Nurses face burnout as hospital staffing shortage continues
Published 1:30 am Monday, January 24, 2022




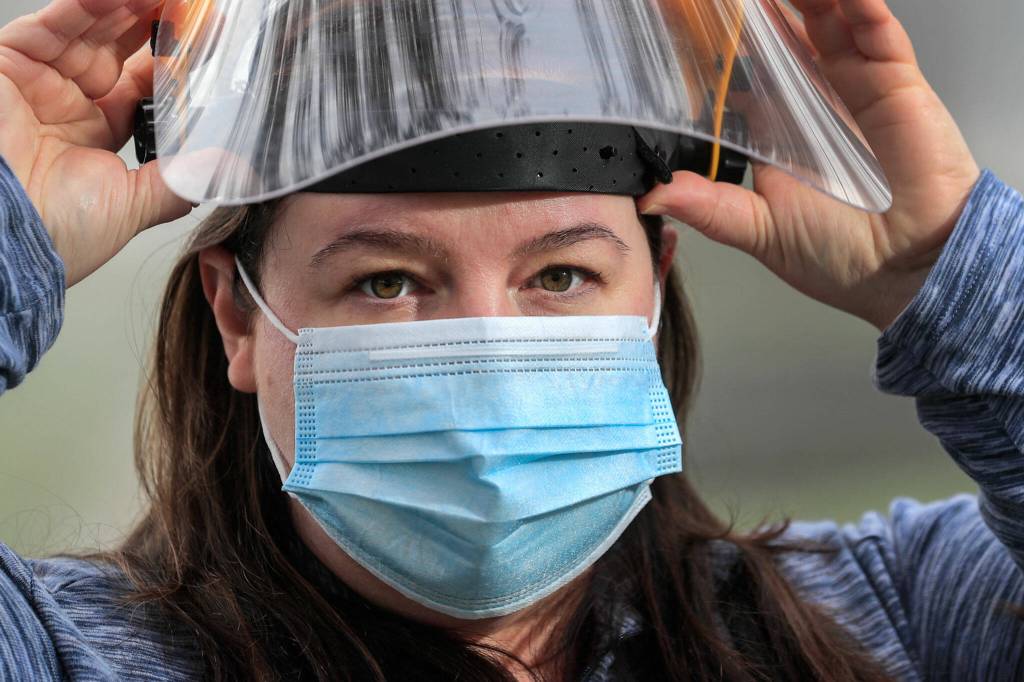
EVERETT — Michelle Roth, an emergency department nurse, is fed up with patients’ rude comments and having things thrown at her.
Roth, a nurse for nearly 20 years, has no plans to leave Providence Regional Medical Center Everett, but her job is only getting tougher.
Hospitals are struggling to hire and retain staff, as the omicron variant surges and the pandemic continues. Nurses are exhausted and traumatized, Roth said. They’ve lost coworkers to burnout or better-paying jobs as travel nurses. Some are temporarily quarantining because they caught COVID.
More than a dozen health care workers from hospitals and clinics in Snohomish County said the public’s anger has made their jobs more challenging. Nurses and medical assistants described patients that threw objects at them, flipped them off or hit them.
Kelley Phan, a charge nurse at Providence, said more than a dozen nurses in her department have quit over the past few months.
“It feels like there has been a mass exodus in the last two to three months,” Phan said. “As nurses, you become family with the people that you work with. It’s like seeing your family leave. But I get it. I don’t blame them.”
Many of the nurses Phan works with are new to the profession.
“I know what nursing can and should be,” Phan said. “But the newer nurses — not so much — this is all they know. And it’s a lot.”
Unions representing more than 71,000 of the state’s health care workers polled members in December. Nearly half said they were likely to leave health care in the next few years. More than 70% cited short staffing as a reason.
The Washington National Guard arrived Friday morning in Everett, after the governor deployed them to help four emergency departments in the state. The governor also ordered hospitals to postpone non-urgent surgeries.
Lawmakers in the state House and Senate are considering legislation that would limit the number of patients assigned to a nurse. Hospitals would face hefty fines if they violated worker protections for medical staff or failed to meet the new standards.
“Obviously hospitals don’t like that,” said Sen. June Robinson, the Everett Democrat who sponsored SB 5751. “They don’t like being regulated in that way. So I think we, as a Legislature, have held off sort of in deference to the hospitals, hoping, assuming they would do the right thing. Years and years go on and it just gets worse and worse.”
Washington State Hospital Association CEO Cassie Sauer recently voiced opposition to the companion bill, HB 1868, at a House Labor and Workplace Standards Committee hearing.
“We agree that more needs to be done for the health care workforce, but we strongly disagree that this bill is the path,” Sauer said. “… It will deepen the staffing crisis in other areas of the health care system and, worst of all, it will undoubtedly lead our hospitals to delay or deny care to many who need it.”
Providence Northwest attributed its hospital’s staffing shortage to a large number of patients who need long-term care.
“We have well over 100 patients in our hospital who are medically ready for discharge, but have no safe and appropriate place in the community to be discharged to,” Providence spokesperson Casey Calamusa emailed The Herald. “For us in Northwest Washington, this is the primary driver of our staffing challenges.”
Maria Goodall, a vascular ultrasound technician at Providence, helped negotiate three of her union’s most recent contracts with Providence. Increasing and retaining staff is a concern at every negotiation, she said.
“It’s definitely a difficult process to get approval for increasing staff,” Goodall said. “My concern is that they don’t always evaluate the things they can’t see. They measure our productivity by what we do in a day, but I don’t think they measure what we didn’t do.”
Goodall said she used to wait about 15 minutes for the hospital’s Transport Team to move patients. Now, it’s more like 45 minutes to an hour. She waits up to two hours on bad days.
Lori Young, a float nurse, said Providence pages her about critical staffing levels every day. The hospital offers a bonus for working extra shifts, but she can only work so much overtime.
Suspending surgeries helped staffing levels, Young said. It freed up more hospital staff for floors that desperately needed them. Only some staff can take patients, though.
“A lot of the surgical nurses have only been surgical nurses,” Young said. “They don’t know how to do floor nursing.”
Nurses can technically decline patient assignments. If the nurse doesn’t feel qualified, another nurse takes the patient. However, that only means more work for the next person, float nurse Julie Bynum said.
“We all have way too many patients,” Bynum said. “It’s unsafe for everybody there, not just me. … Who is going to take care of that patient if I don’t?”
Roth said nurses feel “beaten down and forgotten,” but the environment isn’t specific to Providence. She hears similar sentiments from nurses across the country.
The public’s attitude toward health care workers has changed drastically, Roth said. They seemed appreciative in the beginning, but the tone shifted about halfway through.
“They almost were targeting us, like, ‘Oh, you’re part of the conspiracy,’” Roth said. “Now it seems like people are just angry.”
Roth said she often hears people attribute hospital staffing shortages to the vaccine requirement. That isn’t the case, she said. She knew one nurse who left because of it. Others qualified for exemptions.
“We don’t have less staff because of them not getting vaccinated,” Roth said. “We have less staff because so many people — probably mid-last year, end of last year — were just like, ‘I don’t even want to be a nurse anymore.’”
Claudia Yaw contributed to this story.
Katie Hayes: katie.hayes@heraldnet.com; Twitter: @misskatiehayes.
Katie Hayes is a Report for America corps member and writes about issues that affect the working class for The Daily Herald.