Editorial: Covid recedes in hospitals, exposing other worries
Published 1:30 am Thursday, December 16, 2021


By The Herald Editorial Board
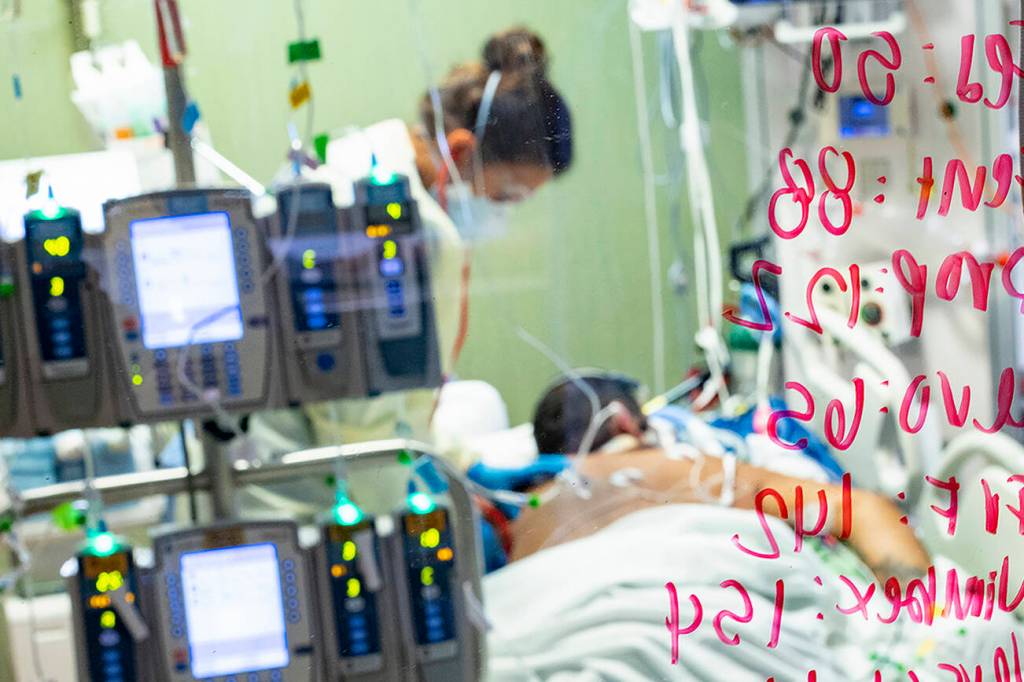
Even as covid-19 cases in Washington state hospitals have subsided — at least for now, with a wary eye trained on the omicron variant — and fewer covid patients are in need of beds, those hospitals are not necessarily seeing their patient counts return to typical levels.
As the wave of covid patients has subsided with the ebb of the pandemic’s latest surge in the state, beds at hospitals and care facilities remain overloaded and nursing and other staff are still overwhelmed by patient care needs, as revealed during a news briefing Monday by the Washington State Hospital Association and other medical officials.
Hospital officials and unions representing nurses and other health care workers are blaming staffing shortages that started before the pandemic’s arrival as well as regulations that are slowing the transfer to long-term care facilities of patients who no longer require treatment and the level of care provided at hospitals.
Dr. Jay Cook, chief medical officer for Providence Regional Medical Center in Everett, told reporters during the briefing that 1 in every 6 beds at Providence’s Everett hospitals was now occupied by someone no longer needing hospital care but waiting to be sent to a long-term care facility.
“We’re having difficulty finding outpatient care facilities to assume their ongoing life needs,” Cook said, as reported by The Olympian. “Many have severe dementia or other challenging behavioral conditions. Some have complex psycho-social, financial or other barriers. Our problem is that these vulnerable but not acutely ill individuals occupy inpatient beds and require the same limited hospital staffing needed for other patients with more severe acute medical problems that need our care.”
The combination of staffing and bed shortages, Cook said, meant that more than 40 elective — but still medically necessary — surgeries were postponed in the past week.
“Providence Everett is facing significant staffing challenges in almost all inpatient departments, including nursing, lab, environmental services and transport,” he said. Those staffing shortages are further complicated by having to provide care for patients who no longer require the hospital’s level of care.
At the same time, three health care workers unions in the state representing nurses and health care workers released the results of a survey that show a significant number — 80 percent — reported feeling “burned out” after nearly two years of the pandemic, with many citing short-staffing, inadequate pay and workplace safety concerns. According to the survey, more than 84 percent reported being very or somewhat burned out. As well, nearly half said it was likely they would leave the health care profession in the next few years.
Those anticipating leaving health care listed having to work at facilities with inadequate staffing as the leading reason — 71 percent — for their dissatisfaction, followed by low pay (53 percent), workplace safety (42 percent) and planned retirement (23 percent).
Those reports from hospital and health care officials and staff are concerning, especially since there’s no clear indication that the current decline in covid patient numbers will continue in this state, as concern grows for a potential wave of infections caused by the omicron variant.
Less than a month after it was first detected, omicron has turned up in patients in 77 countries, including the United States and is spreading “at a rate we have not seen with any previous variant,” a World Health Organization official said at a news briefing.
While the omicron variant may spread more easily, early research from South Africa, among the first nations to identify the variant, link omicron to fewer hospitalizations. Still, the WHO official said, “the sheer number of cases could overwhelm unprepared health systems.”
Provided even a brief reprieve from covid hospitalizations, work should be ramped up on short- and long-term solutions. Providence Everett’s Cook pointed to New York’s use of National Guard units to bolster staffing at long-term care facilities and nursing homes and called for similar funding and staffing supports at state and federal levels.
The state hospital association has called for state lawmakers during their session starting Jan. 10 to consider legislation that would streamline a guardianship process that is slowing transfers from hospitals to care facilities because it is complex, expensive and requires extensive court review. The association also is recommending the state provide higher payment rates for long-term care facilities to improve wages and increase hiring.
And, as the union survey shows, hospitals will need to consider staff and pay increases that will help retain current employees. Union officials are looking for legislation that addresses staffing levels, working conditions and investments in workforce training and development.
At the same time, there’s responsibility for state residents to do everything they can to stay healthy and out of hospitals, in particular, wearing masks where required, maintaining a safe distance in public and getting themselves and eligible children vaccinated, including booster shots.
Even at the peak of hospitalizations and occupation of intensive care units for covid, Washington state hospitals have been able to avoid operating under “crisis care standards,” under which care is rationed with priority given to patients deemed most likely to survive. The state might not be as fortunate if there is another surge. Idaho in September had to implement those standards and ration care statewide until the end of November, but kept the standards in effect longer for northern Idaho.
As the latest covid wave recedes, the pandemic has exposed longer-term problems at hospitals and other care facilities in the state. We may have only limited time to start addressing those problems.