Nursing homes face staffing crunch
Published 1:30 am Monday, February 13, 2023



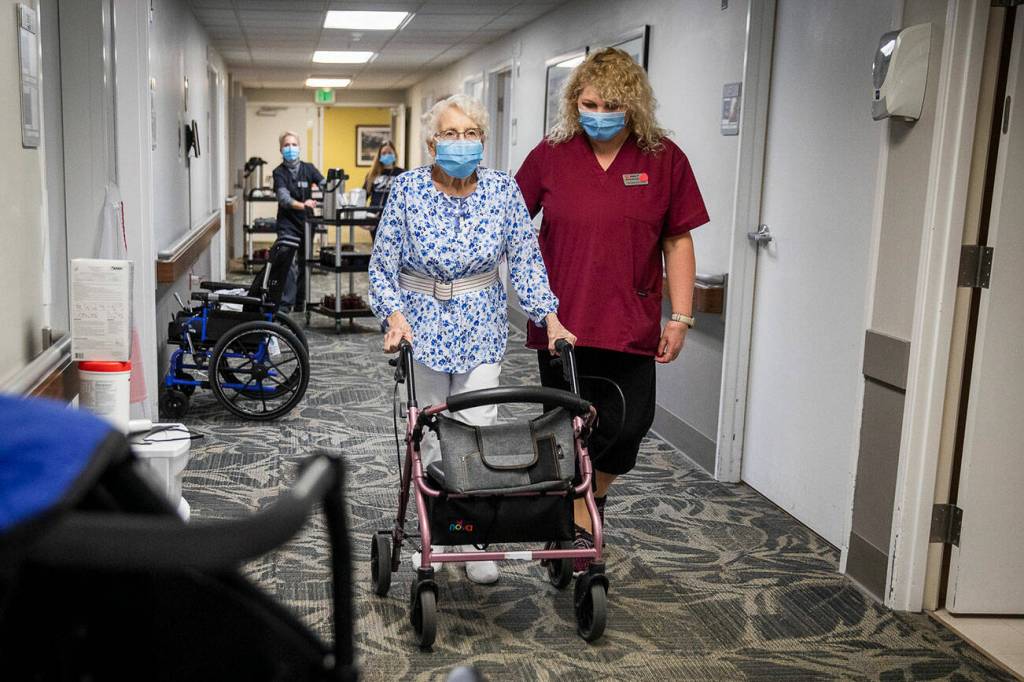
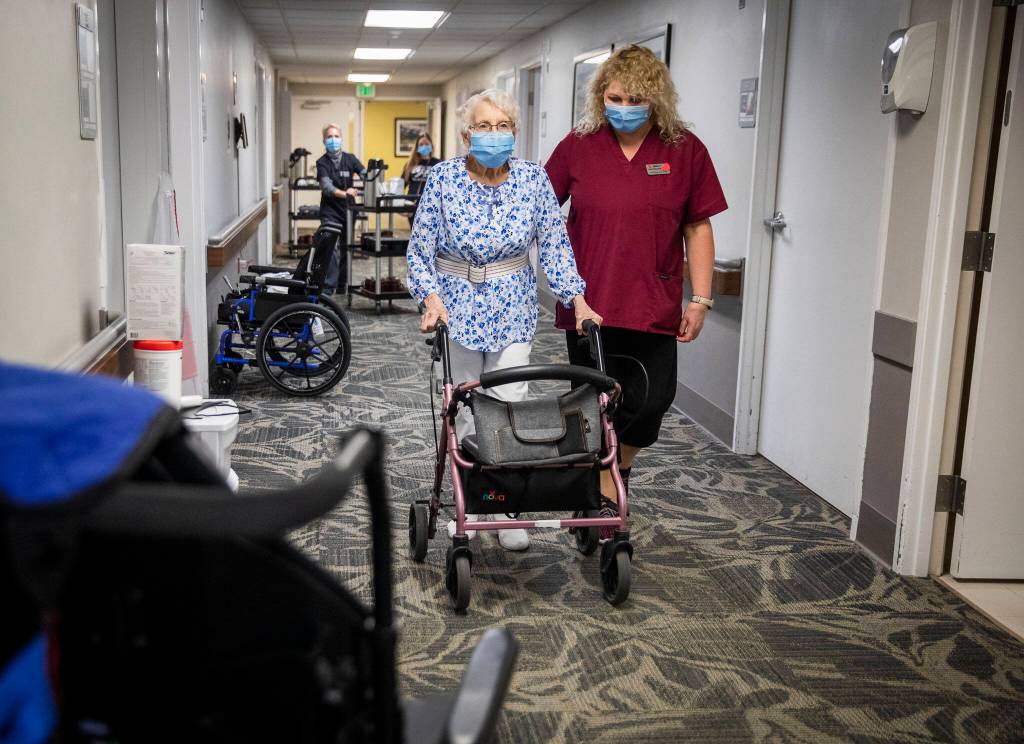
EVERETT — Inside Nightingale Healthcare’s two nursing facilities in Snohomish County, beds and rooms remain empty and patients who need them wait in hospitals or elsewhere.
Those beds are empty at Nightingale, and elsewhere, because of a lack of skilled nursing staff — their “biggest challenge,” said Pete Wolkin, director of operations.
Statewide, about 6,800 of the 19,386 licensed beds in skilled nursing facilities sat empty as of June 2022, according to data analyzed by Carma Matti-Jackson, president and CEO of the Washington Health Care Association. That’s a 35% vacancy rate.
A big problem is money — not enough to recruit and retain qualified staff. State lawmakers are considering several bills to bolster the nursing staff in long-term care facilities, so that more of the licensed beds could be used to care for patients.
Long-term care includes in-home care, adult family homes, assisted living and skilled nursing facilities. In skilled nursing specifically, patients might stay for a few weeks, or a few years, depending on their care plan. They receive around-the-clock nursing care.
One bill in particular, Senate Bill 5526, would increase the Medicaid rate that the state pays to skilled nursing facilities. Medicaid is a major payer for the long stays.
At a hearing on Thursday, bill sponsor Sen. Kevin Van De Wege, D-Sequim, said: “Often times nursing homes are having empty beds not because there’s not people to fill them, but because they don’t have the staff to work them.”
Skilled nursing facilities in Washington state lost more than $600 million in the past five years from caring for Medicaid patients, Matti-Jackson found, using data from the Department of Social and Health Services.
The proposed Medicaid payment rate in the bill changes a complicated reimbursement methodology, taking into account patient needs and the higher operating costs in King, Pierce and Snohomish counties relative to the rest of the state.
“Medicaid doesn’t pay enough for any building to be full of long-term care patients,” said Tracey Jaeger, director of nursing services at Nightingale. “You couldn’t afford what we pay staff now, you couldn’t afford the level of care that people need. Acuity has really, really gone up in the 12 years that I’ve been in long term care.”
After the bill resets the Medicaid rates, the bill requires that they keep up with inflation.
State Sen. Marko Liias, D-Everett, said providers need that predictability of a change in law, rather than a new budget item every one to two years. Inflation won’t eat away at annual adjustments, and providers can plan ahead on staffing and investing in facilities.
“Giving that certainty ensures that we’re going to get facilities that will last for the long-term, and meet the needs of patients. This certainty is critical,” Liias said.
But, Jaeger said, “if you can’t get the employees to take care of the people, you just can’t make it happen.”
A few recent trends have led to the nursing staff shortage at Nightingale Healthcare’s seven nursing facilities in Washington and Oregon.
A number of Nightingale staff, at or close to retirement, left in the beginning of the COVID pandemic, Jaeger said.
And since then, they can’t recruit enough staff, as the pandemic and overall health care workforce shortages have thrown wrenches in the pipeline. Nursing education programs couldn’t send students to long-term care facilities during the earlier part of the COVID public health emergency.
Those facilities, like Nightingale’s View Ridge in Everett, now compete against hospitals for staff like licensed practical nurses. Since the pandemic, acute care hospitals have started hiring new registered nurse graduates, and also offering moving and hiring bonuses, Jaeger said.
Wolkin, director of operations, said they could have higher occupancy than they have now. But that would depend on the ability to staff appropriately based on patients’ level of need.
Data and stories from providers suggest that the low occupancy results from an inadequate supply of staff. From 2019 to 2021, Washington skilled nursing facilities more than doubled their spending on temporary or “contracted agency staffing” — from $37 million to $76 million, according to cost report data analyzed by Matti-Jackson.
Skilled nursing facilities have minimum staffing requirements in Washington. A registered nurse must be on duty every hour of every day, and facilities must provide a minimum of 3.4 hours of care per resident day.
They have paid more for contracted staff during the pandemic because of the law of supply and demand. But the government does not reimburse for extra expenses beyond what a facility would pay a regular employee. So, Washington skilled nursing facilities did not get reimbursed $31.3 million in 2021 for contracted labor.
Hospital leaders statewide, including from Providence in Everett, have cited the backlog of “difficult to discharge” patients as one reason for overcrowded emergency departments. These patients are medically ready to leave the acute care setting, but still need support, some in a long-term care setting.
It could become even more difficult to find a bed and appropriate care for seniors and people with disabilities as the state phases back in minimum staffing requirements. It had relaxed those requirements during the COVID public health emergency.
In addition, Matti-Jackson, from the Washington Health Care Alliance, has warned for years about the looming staffing challenges in long-term care. She now speaks for over 500 member facilities.
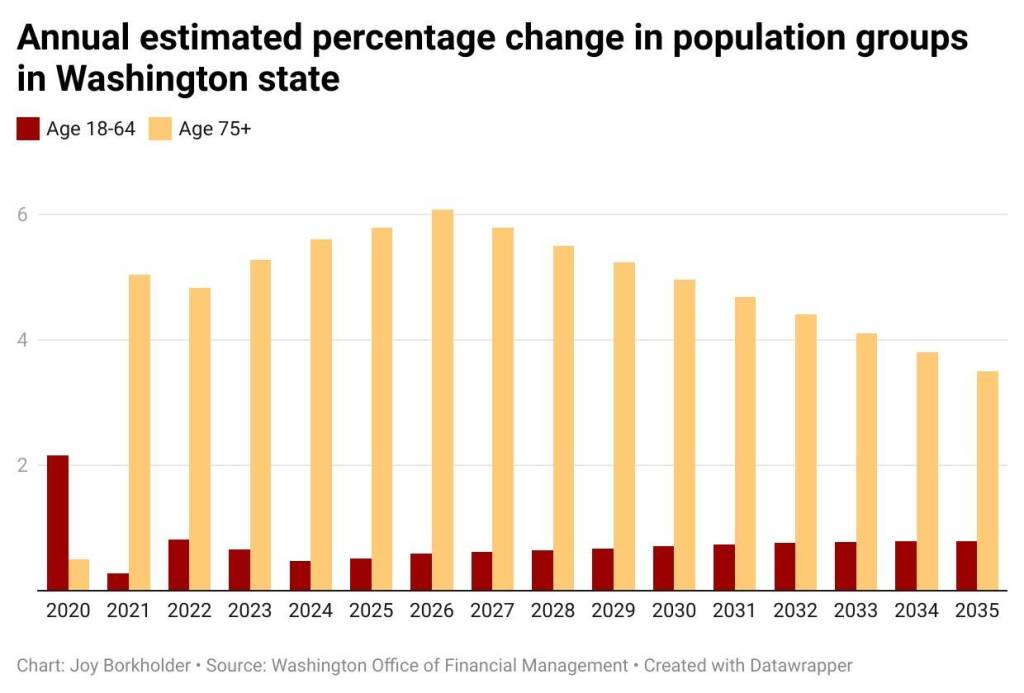
In Washington state, the number of residents age 75 and older is projected to grow an average 5% per year from 2020 to 2035, according to state data. Meanwhile, the number of working adults, age 18-64, will grow by less than 1% per year. The result: a widening gap in the overall workforce and the demand for long-term care.
And nursing staff in long-term care earn less than their counterparts in other settings. For example, a certified nursing assistant in long-term care earned on average $16.61 to $18.03 per hour in 2021, according to federal data. They could have earned several dollars more in a hospital, outpatient setting or staffing agency.
During the pandemic, a temporary increase in the Medicaid rate helped nursing facilities raise wages for some low-wage workers by up to $4 per hour, according to the state budget. Senate Bill 5526 makes this change permanent.
And the bill would require a facility to spend a minimum percent of any rate increases to increase wages for the low-wage direct and indirect care workforce — nursing assistants and housekeepers for example.
Adam Glickman, secretary-treasurer of SEIU 775 — a union that represents 45,000 workers in home care and skilled nursing facilities — said this part of the bill is needed for accountability and transparency. The union has heard from some non-union workers that in the past, reimbursements rates have increased while wages stayed flat.
“I think we just want to make sure that, and I think a lot of legislators want to be sure that, if they’re increasing the funding, that the funding is really going to the place that needs it the most — which is increasing wages and benefits for lower wage, nursing home workers.”
At a legislative hearing on Thursday, over 50 people signed in supporting the bill, including workers and representatives from hospitals, long-term associations and unions. No one opposed it.
Despite the challenges, Wolkin and Jaeger exude dedication and some optimism in this work of caring for patients. The founders of this small, family-owned, for-profit company, named it after Florence Nightingale, the “mother of modern nursing practice.” The company’s leaders “believe in the power of an environment to help people heal themselves,” Wolkin said.
“Seeing the residents, seeing them flourish, and seeing them happy and healthy, or as healthy as they can be, gives me a lot of hope. They’re a big part of our community and our society, and we need to treasure them,” Wolkin said. “And the staff showing up every day, even through the pandemic — unbelievable trials and tribulations — and showing up day after day, gives us a lot of hope. We just want to reward them.”
The Herald will continue to report on access to long-term care. If you would like to share your story as a patient, worker or family member, please get in touch.
Joy Borkholder: 425-339-3430; joy.borkholder@heraldnet.com; Twitter: @jlbinvestigates.