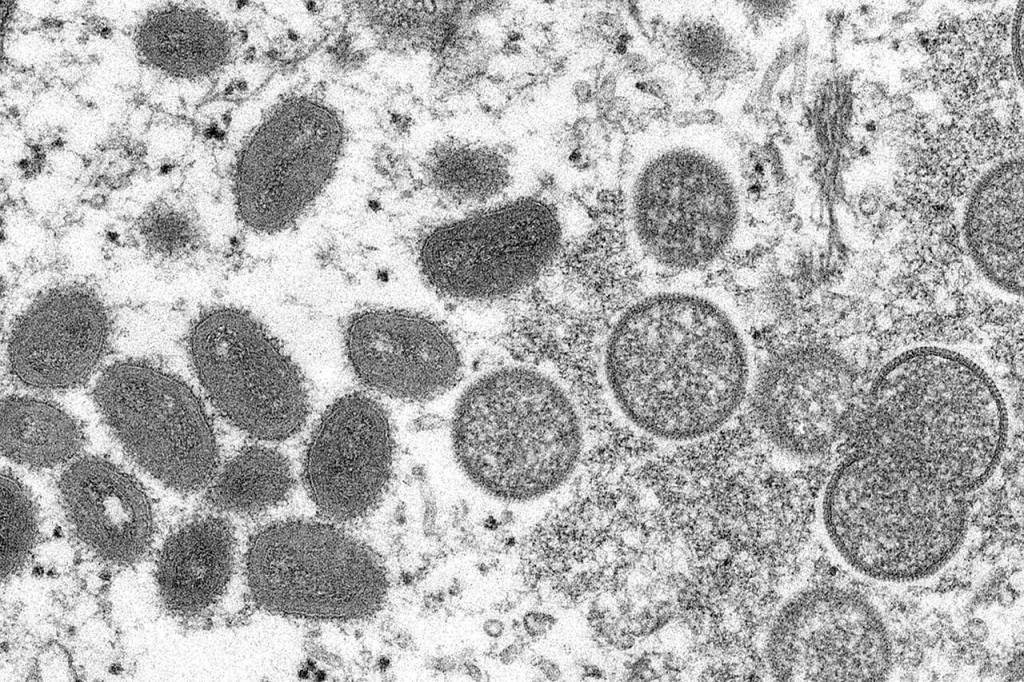
Monkeypox vaccine supply ‘severely limited,’ but more is on the way
Published 1:30 am Saturday, July 23, 2022


EVERETT — For months after the first COVID-19 case in the nation was confirmed in Everett in 2020, little was known about the new virus and how it spread. Guidelines were constantly changing. Tests were in short supply, some were defective and there was no vaccine.
But unlike the novel coronavirus, monkeypox is not new. Outbreaks have plagued West and Central Africa for decades. Scientists have been researching the virus since the 1970s.
“We have a lot more knowledge on monkeypox,” said Kari Bray, a spokesperson for the Snohomish Health District.
In May, the United States reported its first monkeypox case amid a worldwide outbreak. Since then, the country has recorded over 2,890 cases, and as of Friday, over 80 have come from Washington.
As in many places in the United States, the available vaccine supply in Washington is still “severely limited,” according to the state Department of Health. Right now, vaccination supply is very limited and is prioritized for people at high risk of recent exposure to monkeypox. This approach aims to help slow the spread of the disease, particularly for people who may have been exposed but may not have symptoms yet.
This month Snohomish County reported its first two monkeypox cases. Both were men, and their cases were unrelated. Men who have sex with men have accounted for the majority of cases, though anyone can contract the virus through physical contact, according to public health experts. Cases will likely start increasing more rapidly in places that began seeing infections in recent weeks, according to the state health department.
Snohomish Health District Health Officer Dr. Chris Spitters said his agency is trying to contain the spread of monkeypox, whereas the focus of the COVID response shifted to reducing severe illness and death when containment failed.
In a CBS interview on Sunday, former Food and Drug Administration commissioner Dr. Scott Gottlieb said the window to control the spread of monkeypox may have already passed: “We’ve failed to contain this. We’re now at the cusp of this becoming an endemic virus, with this now become something that’s persistent that we need to continue to deal with.”
Doctors, epidemiology experts, LGBTQ activists and politicians including Sen. Patty Murray have criticized the federal government for not responding quickly or aggressively enough. Testing shortages and delays were widespread during the first month of the outbreak in the United States, when testing was only being performed at a limited number of government labs.
Teresa McCallion, a spokesperson from the Washington State Department of Health, said the state has been able to meet testing demand.
Meanwhile, demand for vaccines has far outweighed supply. When the outbreak began, the United States’ national stockpile only contained 2,400 doses of the Jynneos vaccine, which is designed as a two-dose course. At the end of June, the Biden administration announced it would distribute a total of 56,000 doses to regions throughout the country based on how many cases each reported. On July 8, Washington received 398 two-dose courses of the vaccine.
Since then, the federal government has distributed almost 200,000 vaccines to states. Around 800,000 more doses are expected to arrive in the country this summer. Millions more doses could be delivered by mid-2023.
“The limited amounts of vaccine that we have now may not contain the outbreak on its own,” said Sharon Bogan, spokesperson for King County’s public health department.
People don’t always know who they may have exposed or how to contact them, Bogan said. That limits the effectiveness of contact tracing. So pre-exposure vaccination is vital.
“I’m hopeful that as we get more vaccine coming in from the federal level in the weeks and months ahead, that the vaccine will be able to make a difference,” Bogan said.
Before this year, the largest monkeypox outbreak in the United States involved around 70 cases.
“Clinicians on the ground may have never seen a monkeypox case, even a month ago,” Bogan said.
As of Friday, all but five states had reported monkeypox cases.
On social media, some people have questioned why vaccines haven’t been made available to high-risk groups through vaccination clinics in the Seattle area, as they have in some other major cities where monkeypox is spreading.
Lessons from the COVID pandemic will help guide the state’s monkeypox vaccine rollout. A first come, first served approach may not reach those with limited access to care, such as those who are uninsured and communities of color, Bogan said.
Meanwhile, San Francisco and New York City have faced rollout issues including long lines and overwhelming demand. Bogan said King County’s public health department is seeking out providers, clinics and organizations to partner with to reach different demographics.
Bogan stressed the importance of individual efforts to reduce the spread. These include practicing safe sex and avoiding close physical contact with anyone who has open wounds, sores or rashes.
Natalie Kahn: 425-339-3430; natalie.kahn@heraldnet.com; Twitter: @nataliefkahn.