Time matters: Everett gains close-to-home care for stroke patients
Published 6:00 am Monday, June 14, 2021
If you’re experiencing a stroke, time matters – the sooner you receive care, the better the outcome.
Now, rather than having to travel into Seattle to get the care they need, our north region residents benefit from exceptional expertise and care right here at home. And that’s significant – for patients and their families.
The welcome change comes from a new 24/7 endovascular thrombectomy program for acute stroke patients launched earlier this year by Providence Regional Medical Center’s Neuroscience Institute.
“Time is brain,” says Martin C. Holland, MD, chief of neurosurgery and medical director of neurosciences development. “By offering endovascular thrombectomy for stroke patients at Providence Regional, and not having to transfer patients to Seattle, we can start treatment 60 to 90 minutes earlier. Patients also get to stay near their families and work with providers who continue to care for them locally.”
The program is the latest in a four-year initiative to grow the neurosciences program to meet the expanding needs of patients – while 80 patients were sent from Everett to Seattle for intervention or neuro critical care monitoring in 2020, patients now receive care in their own community at Providence Regional.
This addition of new, advanced technology and expertise provided in partnership with the Swedish Neurosciences Institute has advanced Providence Regional’s already-strong stroke program to include the latest neurointerventional capabilities.
“Our partnership has created a very specialized skill set, available at Providence Regional around the clock with a host of new options for stroke treatment,” says Dr. Holland.
Time + technology to improve outcomes
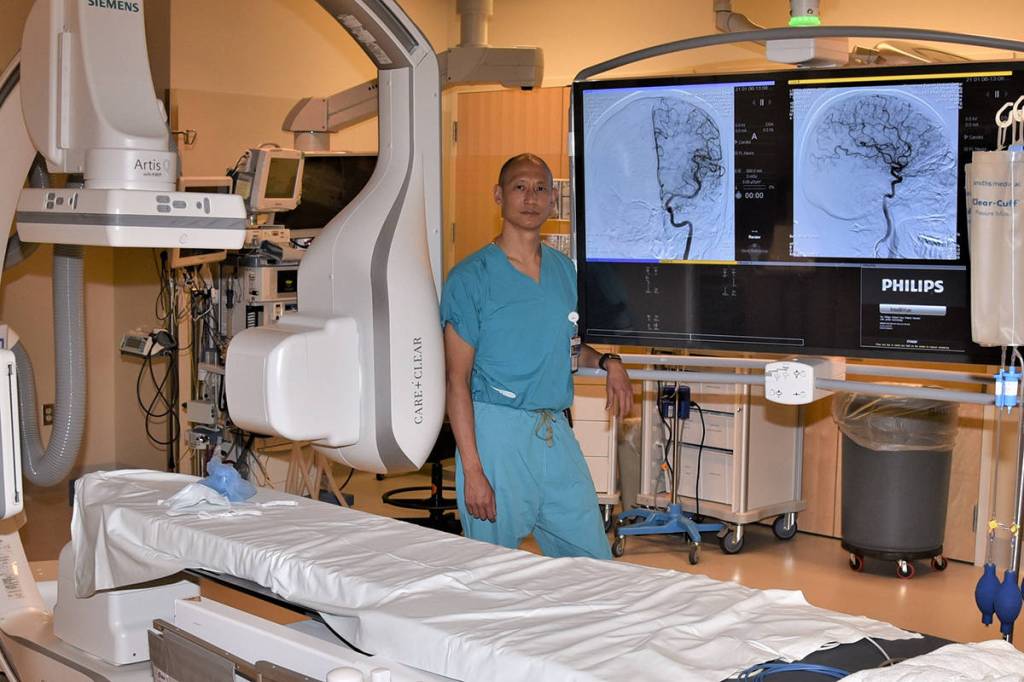
Provided with support from the Providence General Foundation, a neurointerventional surgical suite equipped with biplane minimally invasive technology is specifically designed for the diagnosis and treatment of neurological disorders, such as stroke.
This advanced technology offers patients less risk of bleeding and infection as well as a faster recovery compared to traditional brain surgery.
“When patients are brought in with a stroke, a neurologist must urgently decide between two main treatment options,” explains Tarvinder Singh, MD, neurology and stroke medical director.
“The first option is a clot-busting medication given through IV to a stroke patient presenting within 4 ½ hours of symptom onset. The second, much newer treatment – mechanical thrombectomy – can be offered up to 24 hours from symptom onset. This is for a select group of patients with a clot blocking a larger blood vessel in the brain” Dr. Singh says, noting that these larger clots often do not dissolve with medication and cause significant disability.
In the center’s biplane suite, two rotating cameras provide precise 3-D location of the clot in the brain, then the skilled neurointerventionalist team threads clot-retrieval catheters through the blood vessels to remove the clot.
“Stroke comes suddenly and can be devastating for the patient and their families. Emergent stroke treatment saves lives and prevents disability,” Singh says.
To learn more, visit online or call