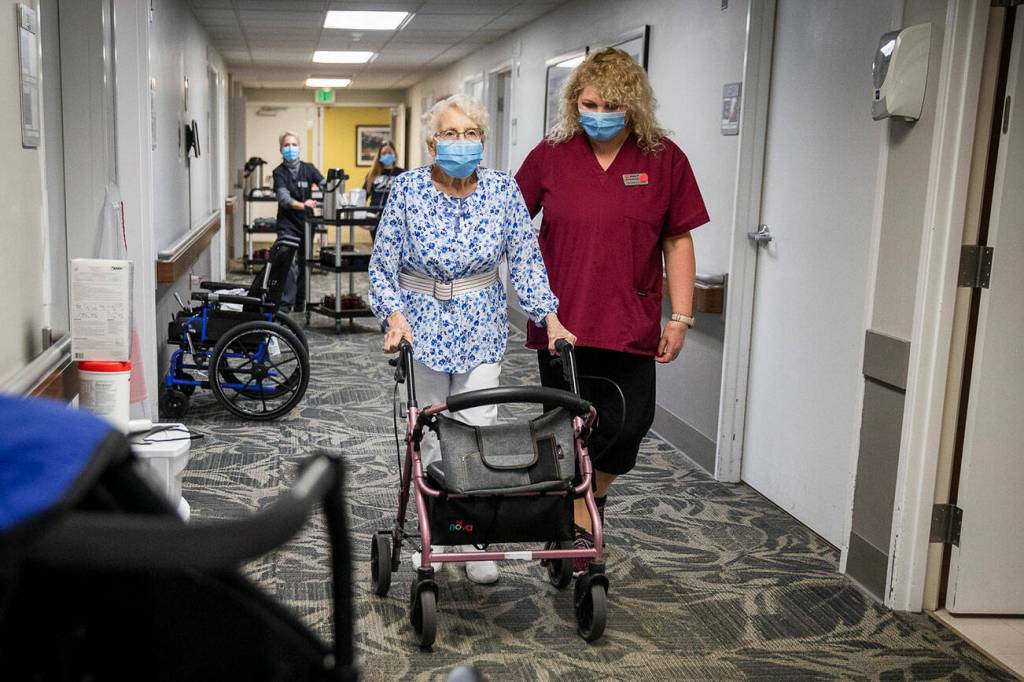
Editorial: Skilled nursing care must remain state budget priority
Published 1:30 am Tuesday, December 30, 2025


By The Herald Editorial Board
Gov. Bob Ferguson, in his budget proposal to the state Legislature, is paring — certainly not partying — like it’s 2022.
Advocates for the state’s skilled nursing facilities and assisted living facilities are hoping state lawmakers can at least shoot for 2024.
The $79 million budget plan Ferguson released last week avoids general tax increases but seeks to fill a $2.3 billion budget hole by cutting some $800 million from state spending, reallocating $880 million from the state’s “rainy day fund” and diverting $570 million from the state’s Climate Commitment Act funds — intended for climate-related and clean energy projects — to cover the state’s working families tax credit.
(At the same time the governor announced support for a “millionaire’s tax,” an income tax on annual personal revenue — and not on net worth — over $1 million. But that support comes with the understanding that — with expected opposition and court challenges even if it were to pass the Legislature this coming session or next — the tax would still be years from gathering any significant revenue for the state and can provide no relief for the state’s immediate needs.)
That leaves the governor and lawmakers to consider cuts, additional taxes or fee increases or a combination, leaving few options that will satisfy many. But with a growing population of baby boomers — 17.5 percent of the state’s 8 million people as of 2023 — lawmakers, as they gather next month for a 60-day session, will need to carefully consider any cuts to the state’s share of Medicaid funding, particularly for those in skilled-nursing facilities and assisted-living centers.
The Legislature addressed that specific need this year when it passed the budget, adopting a plan that beginning in 2026 would have updated the state’s Medicaid reimbursement rates for skilled nursing and assisted living facilities to the wage levels paid by those facilities as of 2024, rather than the 2022 wage level used currently. But that was before Congress passed its so-called One Big Beautiful Bill Act, which is projected to cut $863 billion over the next 10 years from states’ Medicaid funding, a significant loss of support for states that share responsibility for support of those programs.
Among the governor’s suggested cuts was a proposal that would temporarily reduce support for skilled nursing and assisted living facilities back to 2022 levels. Combined with the loss of federal funding, the 2022 funding level would mean a loss of $148 million for those facilities, which care for 13,000 short- and long-term care patients at skilled nursing facilities and another 33,000 in assisted-living facilities, said Carma Matti-Jackson, chief executive of the Washington Health Care Association, which represents skilled-nursing and assisted-living providers in the state.
Even the 2024 level of funding represents $4-an-hour less in what Medicaid provided and what facilities would pay their staff. Clawed back to 2022 levels, the gap will increase to a $13-an-hour difference, Matti-Jackson said.
“So there’s a severe gap between the level of funding that is needed to actually pay for our labor and quality care and what’s actually being provided. And so we’re concerned,” she said in an interview with the editorial board prior to release of the governor’s budget.
Days later that concern ramped up significantly.
“This budget’s attack on our health care system puts our hospitals under increased strain, raises barriers for accessing care in assisted living and skilled nursing, undermines our state’s ability to maintain a high-quality workforce of caregivers and threatens basic maintenance of long-term care facilities,” Matti-Jackson said in a statement last week. “If we cut funding for assisted living and skilled nursing, we undermine the entire spectrum of health care services in our state as people get stuck in hospitals and overload our emergency services.”
Adding to the concern, said colleague Amanda Lanser, executive director for Mountain View Rehabilitation in Marysville, is the growing complexity of nursing care following the pandemic, complexity that increases the dependence on trained and experienced nursing staff.
“After covid, we were continuing to take a lot more complex residents and with the same reimbursement,” she said. “The psycho-social needs of a lot of the residents, even in our local area, it’s definitely shifted a lot, and clinical care needs have become a lot more extreme for the average patient in facilities,” she said.
Lanser, in a recent commentary published in The Herald, warned that many skilled nursing facilities in the state have closed, even before the pandemic, and others now are on the brink of closure because of increased operational costs for supplies and utilities and the lagging state and federal support necessary to attract and retain experienced staff. All while an aging state population threatens to put further strain on skilled nursing and assisted living facilities.
Washington state faces a growing wave of demand for nursing care with an average population of 642 adults 85 years and older for each nursing facility in the state, sixth in the nation after Arizona, which leads the nation with more than 1,050 of those 85 and older per skilled nursing facility, according to U.S. Census Bureau data cited in a report on aging in the U.S.
Currently, Matti-Jackson said, the skilled nursing facilities in the state take in about 40,000 patients from hospitals each year. Between now and 2050, the state can expect the population of residents 85 and older to increase by more than 200,000, about the population of Tacoma.
“As our entire state prepares for a rapid increase in the population of older adults as the baby boom generation ages, we cannot afford to have less skilled nursing care available in fewer areas,” Lanser wrote.
A spokeswoman for the governor’s office, noting the significant funding shortfall that state faces, said Ferguson’s budget proposal is a starting point for the process and his office welcomed counter-proposals from advocates and lawmakers.
That flexibility is well-advised. The governor’s budget proposal should be seen as a baseline from which to start negotiations. But there should also be a baseline of services and spending that must be held as priorities, among them especially K-12 education and the state’s most vulnerable populations.
The state’s elder population, in particular, and those who care for its members are facing a rising tide of demand, costs and complexity, even as Congress has heaped on even greater neglect with cuts to Medicaid, the Affordable Care Act and SNAP food assistance — in order to pay for tax cuts largely benefitting the wealthy — and from the Trump administration’s deportation efforts, which have already driven away a significant number from the direct-care workforce.
The budget work of state lawmakers is never simple; even less so when facing a budget hole. But there remain needs and responsibilities in the state that cannot get by on short shrift.