Getting surgery in Everett? Robots might be helping.
Published 1:30 am Saturday, September 6, 2025








EVERETT — A longtime family practice doctor had to go through knee replacements in both of his legs.
The first time Dr. Charles Chaffee went through the procedure in 2019, it took several weeks to get off of pain medication, which came with side effects and the risk of habituation. The second time, he was off medication in just two weeks, he told The Daily Herald in an interview.
“My wife would tell you that it was an amazing difference because she had to tolerate my recovery both times,” Chaffee said.
What changed? The second time, his surgeon used a robot for help.
Using robots for surgeries, known as robotic-assisted surgery, has been around for years and is by no means unique to Snohomish County. But advancements in the practice, local surgeons said, have brought benefits to both medical professionals and patients.
Doctors use the robotic machines, known as platforms, for a wide variety of important surgical procedures, ranging from joint replacements to cancer treatment. Prices for the platforms can vary, but generally, they are “million-dollar pieces of equipment,” said Payam Mohadjeri, the chief administrative officer for Providence Swedish in the north Puget Sound region.
“You have to invest in technology, you have to give surgeons the tools to practice medicine,” he said.
The idea for robotic surgery started as a military project in the 1970s, said Dr. Brian Fong, the chief of urology at Providence Regional Medical Center Everett who regularly performs robotic-assisted surgeries. The goal was to allow for remote-controlled surgery machines to replace humans in hazardous areas, but the project found little initial success, Fong said.
The practice evolved during the late 1980s when companies began developing robotic platforms for neurological care and for prostatectomies, according to an article in the Cureus Journal of Medical Science. Prostatectomies, a procedure that removes a portion or the entirety of the prostate gland, is a complex procedure that’s difficult for surgeons to undertake. In the past, it required either large open incisions or the use of laparoscopic cameras, leading to procedures that took up to an entire day to complete, Fong said.
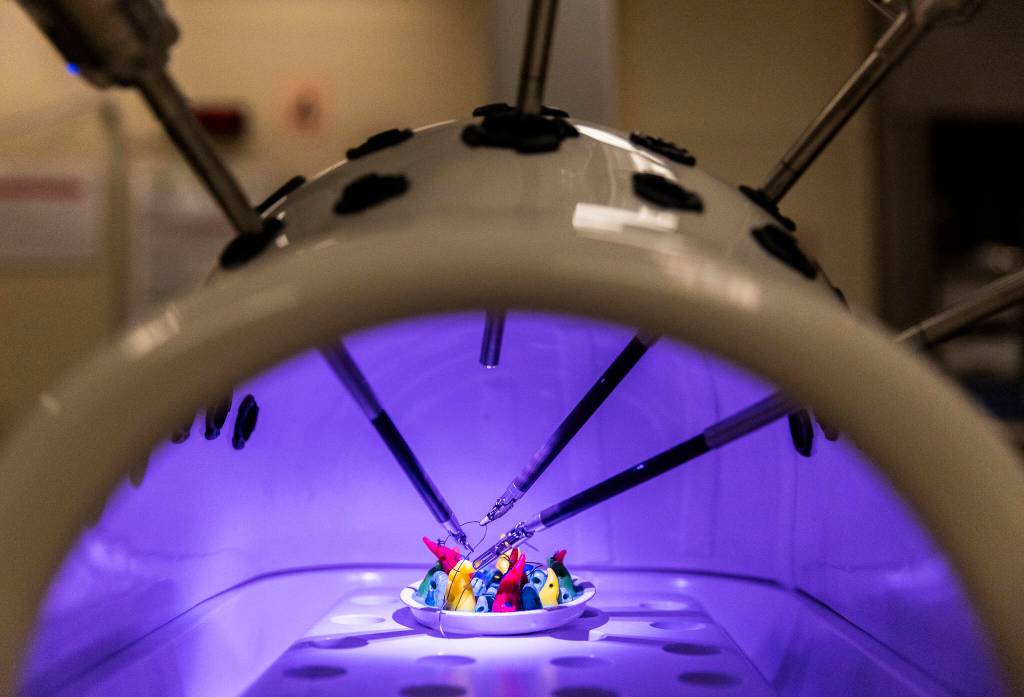
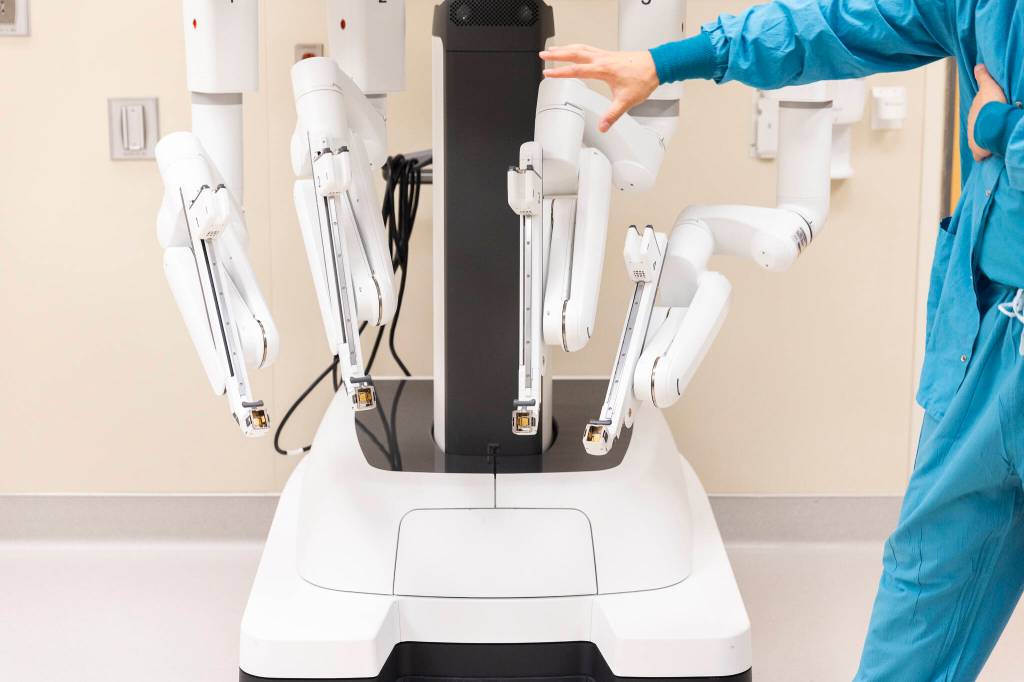
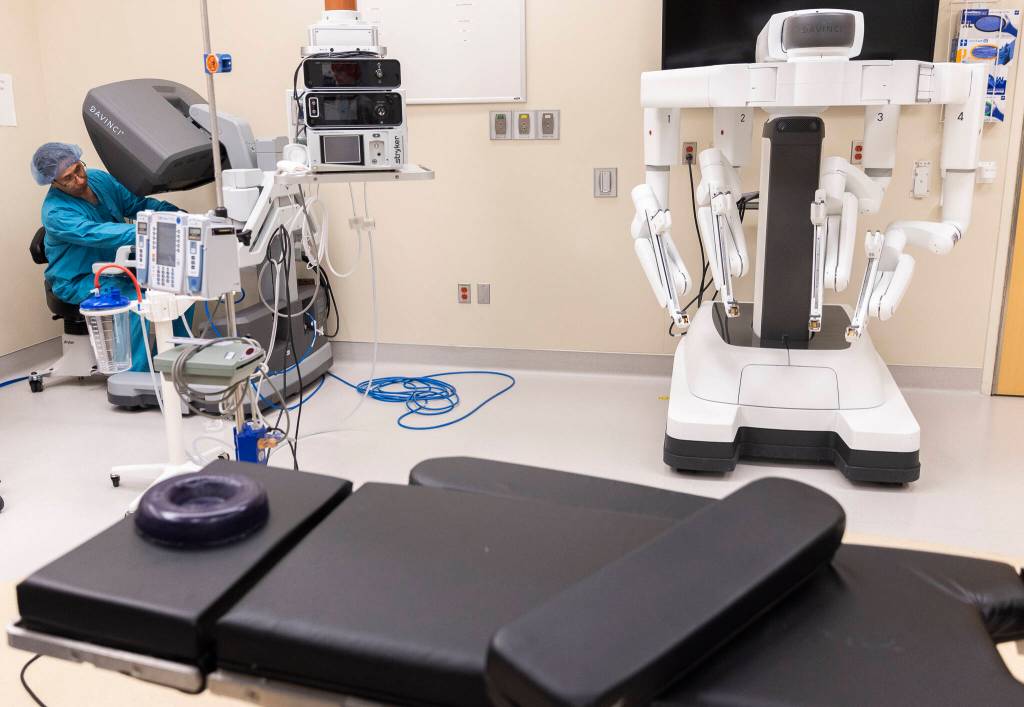
Now, Fong uses a robotic platform — named Da Vinci Xi — to perform prostatectomies. The machine, with its four protruding spider-like arms, can perform complex surgical work with only minor incisions. While operating, surgeons sit at a control seat that resembles an arcade game or a flight simulator, located far away from the actual patient. Surgeons look through a screen while using their hands and feet to control the robotic arms, which perform the surgery. The screen even has 3D vision, so surgeons operating can have depth perception.
“It’s almost like I’m miniaturizing myself in there,” Fong said. “I can do these cases more precisely without having to worry about limited movement.”
All of that precision, along with the small incision sizes, translates to better recovery times and less risk for patients, he said.
“That was the perfect case for using this robot because, in the past, access was next to impossible,” Fong said. “…This translates to certain outcomes, whether it be sparing nerves or quicker recovery because there’s less blood loss, patients are less tired, so there’s a quicker return to work.”
In Everett, Providence Swedish started its robotics program in 2008 with a single platform. Fong performed the first robotic-assisted surgery there that December. Now, the hospital has five in use.
A growing number of surgical professionals use the platforms every day. For many procedures, robotic-assisted surgery is the go-to method.
Dr. Kimberly Costas, a thoracic surgeon in Everett, said about 95 percent of her surgeries now utilize robotic assistance. Thoracic surgeons specialize in surgery of all areas of the chest, apart from the heart.
In the past, Costas said, thoracic procedures required large incisions that allowed surgeons to spread a patient’s ribs open to get medical instruments into their chest.
Her surgeries, which mainly focus on removing nodules, masses or cancer from the lungs or esophagus, are now simpler and safer, she said.
“Because of the flexibility of the robotic instruments and this amazing visualization, we can do very complex thoracic surgeries with this minimally invasive platform,” Costas said. “Before, the complexity of the surgery was really limited by the instruments.”
Dr. Amy BonDurant, a gynecological surgeon in Everett, has seen similar benefits. When performing surgeries to sample lymph nodes or treat ovarian cancer, robotic surgery has allowed for shorter recovery times and allows individuals who need chemotherapy treatment to receive care faster.
“It just tells you how good the technology is, that we feel comfortable to do a surgery like that for people,” she said. “That’s just a world of difference for their healing and getting back onto chemotherapy.”
Robotic-assisted surgeries are currently less common in joint replacements, said Dr. Bill Huang, who performed both of Chaffee’s knee replacements. Most joint replacement in the country still uses mechanical devices that have been commonplace since the 1960s and 70s.
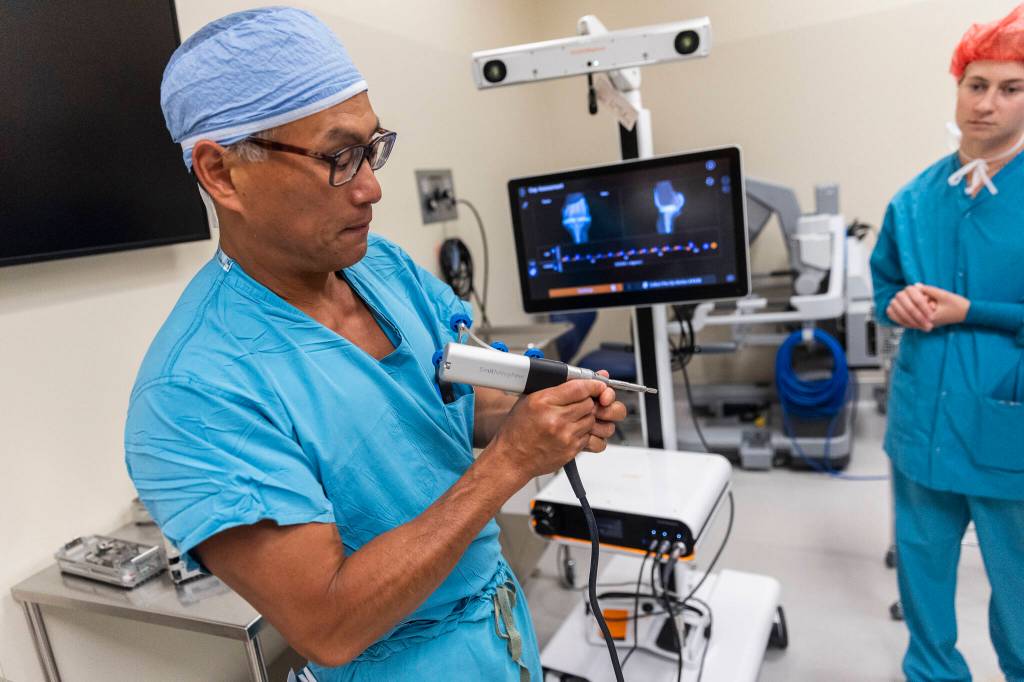
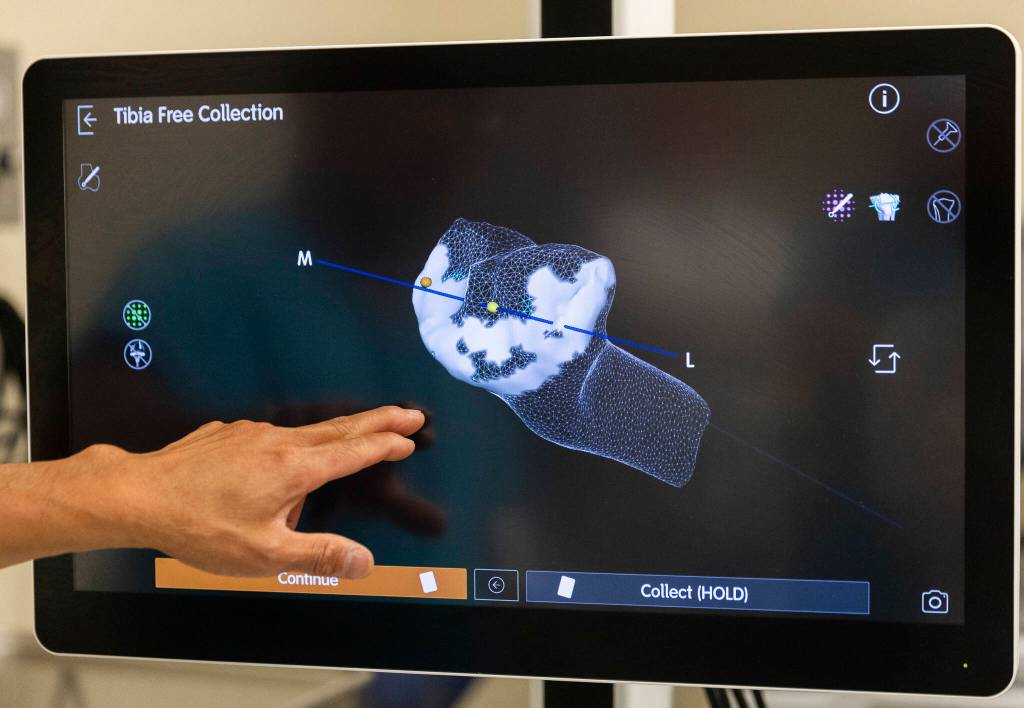
In recent years, however, Huang has utilized a platform known as CORI that allows him to precisely map a patient’s joint to get extremely accurate information about the procedure. To do so, Huang uses a digital pencil to map the topography of the joint, detecting defects in the bone and transferring it to a 3-D model. Through that process, he can then plan out the surgery in advance while also ensuring that implants fit perfectly.
Doing that work before the time of execution, he said, allows for more precision with less damage to surrounding tissue.
“I don’t want to make it sound like joint replacement is minimally invasive or not traumatic to the tissue. It still is, we still have to cut the knee open, we still need to do all the stuff we need to do,” Huang said. “But the data seems to suggest that with this better precision, we’re able to execute with less surrounding soft tissue trauma, and that can translate to a slightly easier recovery for patients.”
For Chaffee, the difference between robotic and non-robotic surgery was night and day. After about three months of recovery, he was already back to going on hikes — recovering at a pace months faster than his previous knee replacement, he said.
“I’m pretty active, so my goals of function are pretty high,” he said. “I’ve been very satisfied.”
Will Geschke: 425-339-3443; william.geschke@heraldnet.com; X: @willgeschke.
Correction: A previous version of this article misspelled Dr. Amy BonDurant’s name. A photo caption also misspelled Geoffrey Bedell’s name.