By Fiza Pirani / The Atlanta Journal-Constitution
Here’s what you need to know about the disease:
What is measles?
Measles became a nationally notifiable infectious disease in 1912, when it was significantly common, according to the Centers for Disease Control and Prevention. The highly contagious disease, also called rubeola, is caused by a virus spread in the air by breathing, coughing or sneezing. Though it can now almost always be prevented with a vaccine, and global death rates attributed to measles are declining, the disease still kills more than 100,000 people a year.
Which groups are most at risk?
Unvaccinated children under age 5 are the most common victims of measles and its potentially fatal complications, along with unvaccinated pregnant women. Generally, anyone who has not been vaccinated is at risk. According to the CDC, 90 percent of people exposed to measles who have not been vaccinated will probably get it.
As for the most at-risk regions, developing countries in parts of Africa and Asia where health infrastructures are relatively weak continue to face measles outbreaks. The disease is also still common in parts of Europe, the Middle East, and the Pacific.
What about the United States?
As a result of high vaccination in the U.S., measles isn’t commonly widespread and is typically a result of international travel. But according to the Mayo Clinic, the average number of annual cases has jumped from 60 between 2000 and 2010 to 205 per year in recent years.
What are the typical symptoms of measles?
According to the CDC, the following symptoms appear one to two weeks after infection:
— High fever
— Cough
— Runny nose
— Red, watery eyes
Once symptoms begin, tiny white Koplik spots may appear inside the mouth before a measles rash breaks out. This rash, which looks like small, red bumps joined together, can spread from the hairline to the rest of the body, spiking an infected individual’s fever to more than 104 degrees Fahrenheit.
How to prevent measles
To protect against measles, ensure you are fully vaccinated. Other steps in prevention include washing your hands often; covering your mouth and nose when sneezing; using hand sanitizer with at least 60 percent alcohol; avoid touching your eyes, nose or mouth and refrain from kissing, hugging or sharing utensils with anyone who is sick.
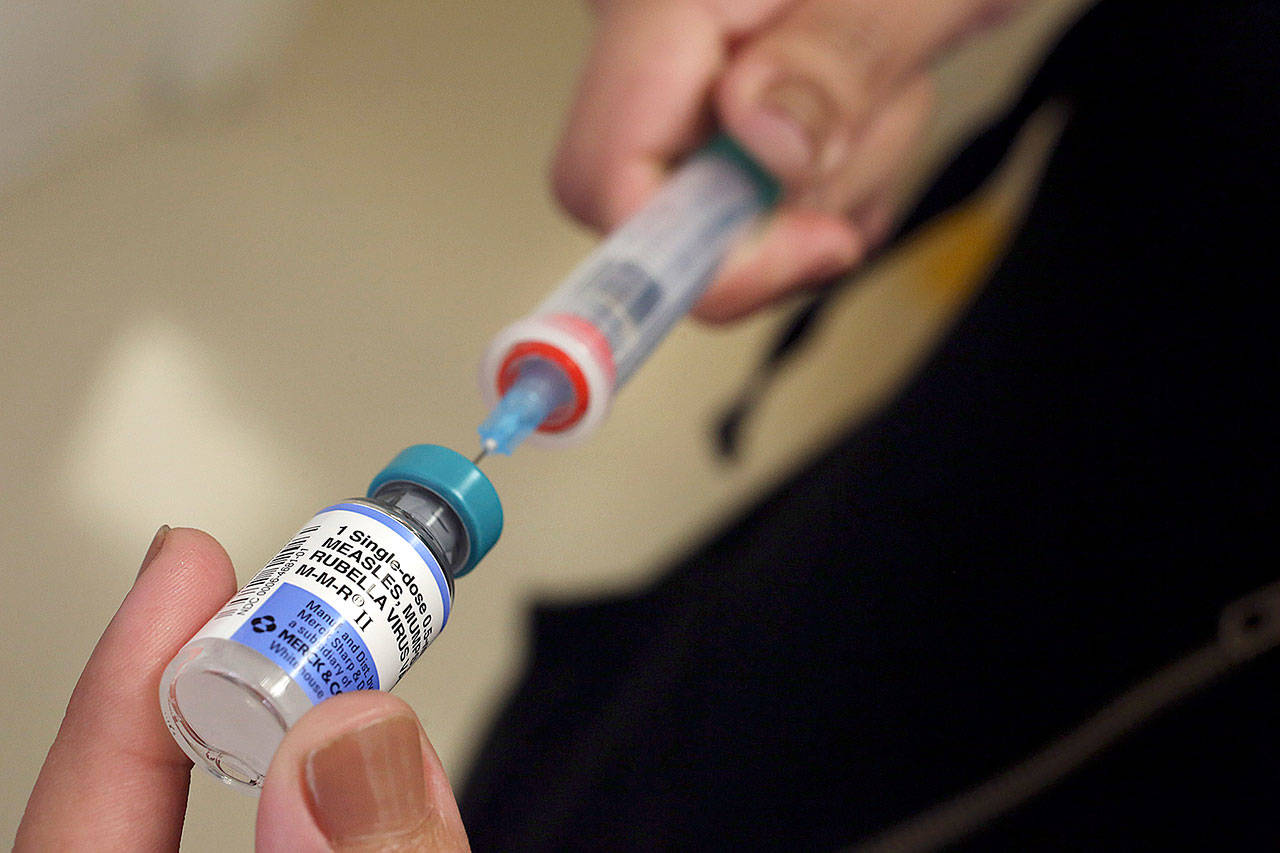
The measles vaccine
Before the measles vaccine was developed, an estimated 3 million to 4 million people in the U.S. were infected each year, according to the CDC. Compared to the pre-vaccine era, the vaccine has led to a greater than 99 percent reduction in cases. In 2000, measles was declared eliminated from the U.S.
The work of scientists John Enders, Thomas C. Peebles, Maurice Hilleman, and others resulted in the Edmonston-Enders strain vaccine, which has been the only measles vaccine used in the country since 1968. This vaccine is typically combined with mumps and rubella (MMR) or a mixture of mumps, rubella and varicella (MMRV), the latter of which is only licensed for use in children 12 months through 12 years of age. The MMR vaccine protects against measles, mumps and rubella, whereas the MMRV vaccine adds varicella (or chickenpox) protection.
Just one dose of measles vaccine is about 93 percent effective at preventing measles. Two doses are about 97 percent effective.
Experts recommend children receive two doses of the MMR vaccine, first at 12 to 15 months of age and again between ages 4 to 6. All teens and adults should also be up to date on vaccinations. Check cdc.gov to learn if you’re one of the exceptions and should hold off on getting a measles vaccine.
If you think you have measles …
Call your doctor immediately. If you’re up to date on your records, you may be immune to the disease. But if you have measles, your doctor will probably recommend staying home for a few days after you see a measles rash coming in.
More online
Learn more about measles at cdc.gov.
Talk to us
> Give us your news tips.
> Send us a letter to the editor.
> More Herald contact information.