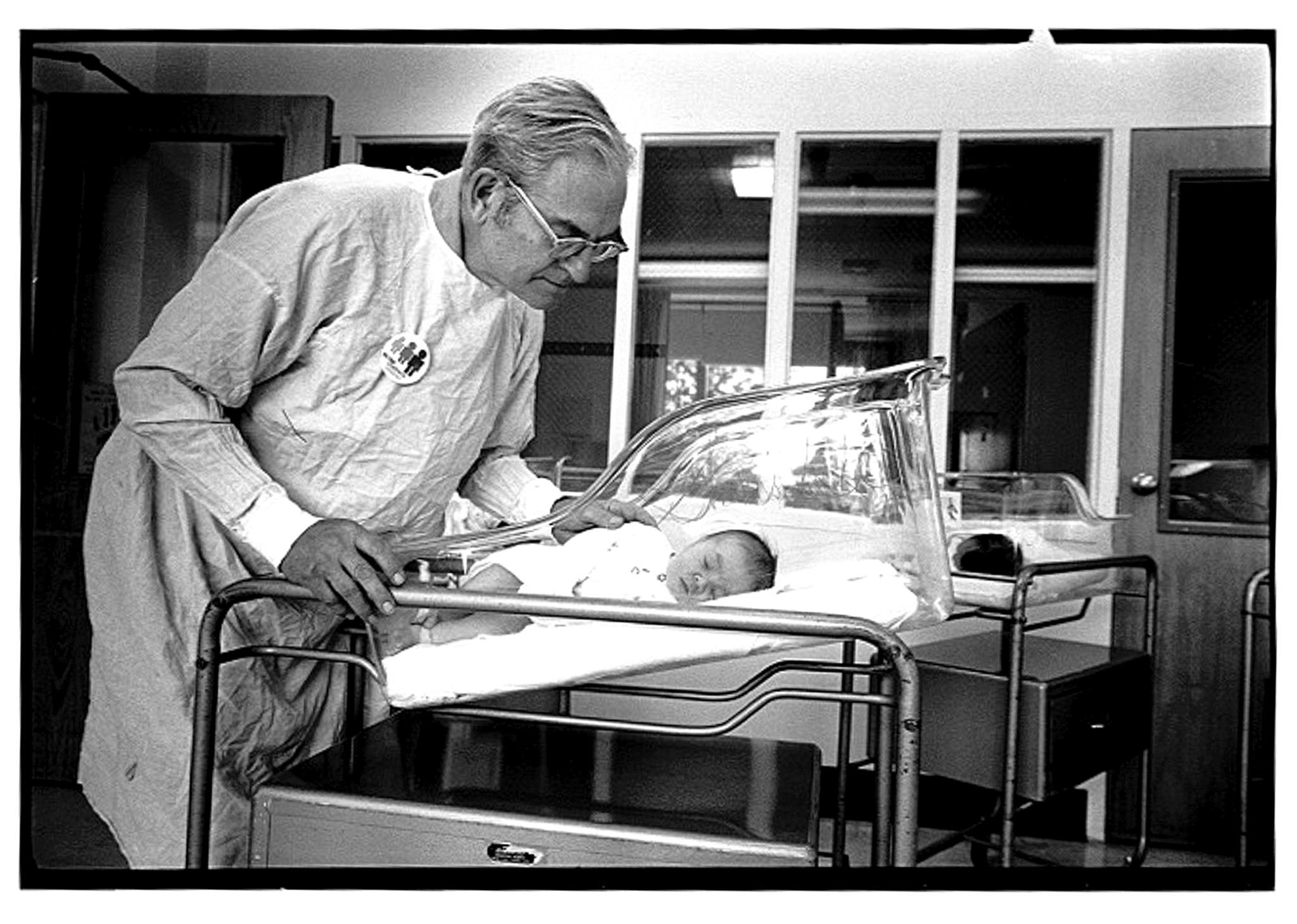
By Patricia S. Guthrie
Special to The Herald
My father makes every baby cry.
Growing up, that’s what I told my friends when they asked what my scientist-doctor-dad had invented. They knew it had something to do with newborn babies, something to do with the letters, P, K and U, and something to do with preventing mental retardation.
The pioneering work of my father, Dr. Robert Guthrie, is known today by three other initials: NBS, for newborn screening. Every infant born in the United States and most developed countries is screened for a variety of potentially deadly or debilitating genetic disorders — conditions that can be treated if caught early.
It takes a tiny prick to an infant’s heel in order to squeeze out the whole blood needed.
Of 88,367 babies born in Washington state last year, 161 were identified with one of 28 life-altering genetic disorders covered by the state’s newborn screening panel. (The $69 cost is part of the hospital’s delivery bill; it will increase to $84.50 next year.)
Five drops of blood
Five spots of whole blood collected at birth, blotted onto filter paper and then dried, comprise the beginning of what is still called the Guthrie Test or the Guthrie Card.
My father’s test, which led to the public health field of newborn screening, was borne from his work more than 50 years ago in Buffalo, New York, on a disorder called phenylketonuria or PKU.
Today, newborns are screened for dozens of genetic disorders within the first days of life, and again at two weeks of age, by state-run programs that send blood spots to laboratories to be analyzed both by human eyes and $400,000 high-tech measuring machines called tandem mass spectrometry. If babies are identified as being positive for one of the screened disorders, they can be successfully treated by strict adherence to dietary intervention, supplemental food or medication.
My father didn’t know his legacy would be screaming babies when he set out to find a simple way to identify PKU, an inherited disorder.
PKU leaves newborns unable to metabolize an essential protein called phenylalanine, which builds to toxic levels in their brains as they consume mother’s milk or standard formula. By the late 1950s, other scientists had unraveled the mystery of the PKU disorder and created a remedy: a low-protein diet and supplemental formula. The remaining challenge, however, was how to identify infants with PKU in their first weeks of life before they suffered irreversible brain damage.
PKU is considered a rare disorder that strikes about one in 10,000 babies. Before newborn screening, PKU was usually diagnosed only after babies failed to develop properly. My father was perfecting the PKU test when he received a phone call from my aunt, who said, “I think my daughter has been diagnosed with what you’re working on.”
Born in 1958, my cousin’s diagnosis of PKU at 18 months came too late to prevent profound intellectual disability. At that time, my parents were also involved in creating support systems for the developmentally disabled because their second son, John, also was mentally retarded, although the cause was never determined.
Expensive ‘diet for life’
Forty years ago, Jennifer Taylor Christenson of Everett was one of those newborns identified with PKU. Her diagnosis was not a shock to her parents, as it usually is, because her older brother also has PKU. Having two children who needed the same low-protein regiment actually made meal planning easier for the family.
But things became more difficult for Jennifer as an adult. She struggled to follow her doctor’s instructions to remain on the “diet for life,” mainly because of the cost of the protein substitute supplemental formula. (Insurance companies often drop coverage of such “medical foods” once a child becomes an adult; coverage varies state to state.)
Decades ago, it had been standard practice to allow PKU patients to consume a “normal” diet as they aged. But after reports of women with PKU giving birth to developmentally disabled children, research showed high phenylalanine levels continued to adversely affect brain function in adults, and could do damage in the womb of pregnant women with PKU.
The “diet for life” recommendation is now viewed as vital for adults with PKU in order to sustain their “equal chance at life,” the mantra of my father about the core value of newborn screening.
But insurance companies — and some legislatures — have yet to get on board.
“I lived in Oregon for 15 years of my adult life, where the medical foods coverage is wonderful,” Christenson said. “I had coverage for both food and formula there. It is state mandated there that insurance covers both. I moved back to Washington state in 2012, and have been fighting for coverage of my formula since.
Like others living with PKU, Christenson must constantly monitor her phenylalanine levels, known as phe levels, through blood work. Now pregnant with her second child, Christenson said she’s kept her levels steady despite the out-of-pocket expenses ballooning to $40,000.
“The formula is not just important, it’s a necessity for a normal, healthy, life,” she said.
Proposed federal legislation called the Medical Nutrition Equity Act that requires public and private insurance to cover formula and other medical foods has yet to gain wide support in Congress.
Legislating health
Universal newborn screening has spared tens of thousands of children worldwide from the fate of developmental and physical disabilities and early death. It’s recognized as one of the most successful and cost-effective programs of public health.
The March of Dimes honored my father on the 40th anniversary celebration of his first newborn screening test, saying its success “has brought extraordinary advances in the health of babies.” Dr. Gary Goldbaum, director of the Snohomish Health District, cites newborn screening and immunizations as “two important public health tools to improve lives and reduce health care costs.”
On the 50th anniversary, a tribute featuring children from every state who were saved by newborn screening took place at the U.S. Capitol, where the Association of Public Health Labs released its book, “Newborn Screening: How One Simple Test Changed Lives, Science and Health in America.”
But the idea of a government-sponsored test that all hospitals were required to offer to every newborn wasn’t warmly received when my father pitched the idea. In the early 1960s, health mandates didn’t exist. The government didn’t tell you to buckle up in your car, didn’t care if you wore a helmet while on a motorcycle (and certainly not on a bicycle), and didn’t label alcohol or cigarettes as dangerous. Back then, many doctors and dentists smoked and were used as role models in cigarette advertisements.
The American Medical Association initially rejected the PKU test, saying research failed to support the need for a universal screen. The organization also didn’t want state governments to start meddling in medicine.
Casting a wide net
Of the 4 million annual births in the United States, about 6,400 newborns benefit from newborn screening’s early detection, according to a 2008 Centers for Disease Control and Prevention report. Some of these disorders are quickly fatal if not found immediately, said Megan McCrillis, Health Services Consultant, Washington State Newborn Screening program.
“Galactosemia is very life threatening,” she said. “The infant can’t digest the mother’s milk and the baby goes into metabolic crisis. This is one of the scariest conditions we can see on a screen.”
Other conditions may not affect a child immediately but will result in failure-to-thrive complications. Over the years, many of the disorders added to the newborn screening panel came after a breakthrough in treatment.
Cystic fibrosis (CF) is one example. The disorder, which affects breathing and digestive function, is caused by a genetic mutation. Before 1960, infants born with the CF died within months. New enzyme and other treatments greatly increased life span. CF was added to newborn screening in 2000 after research showed that immediate detection would further improve health. About 10 to 12 infants are found with cystic fibrosis in Washington every year.
Newborn screening has not been without controversy. Because each state health panel decides which conditions will be analyzed, babies born in one state with a rare condition could die while those born in a different state thrive because the condition is found at birth.
In 2006, a consensus was reached by federal, state and non-profit organizations to recommend screening for 29 core conditions and 25 secondary targets as a national model for state screening panels. The Recommended Uniform Screening Panel has since been increased to 32 core conditions and 26 secondary targets. The RUSP was initially reviewed and accepted by the Secretary of Health and Human Services’ Advisory Committee on Heritable Disorders in Newborns and Children.
But as genetic and technological advances continue, so does the heartbreak of “newborn screening roulette.” Stacey and James Barrett of Oregon experienced that inequity six years ago.
Their fourth child, a son named Liam, died of severe combined immunodeficiency, commonly known as bubble-boy disease. Infants with SCID are unable to fight off infections. But detecting the disorder through newborn screening, combined with a bone marrow transplant before 3 months of age, increases survivability by 95 percent, research has found.
Liam Barrett’s SCID wasn’t diagnosed until 5 months of age — after he’d been hospitalized several times for severe infections. Despite a bone marrow transplant, his lungs were ravaged from fighting infections and he died at 8 months. His parents testified before an Oregon newborn screening committee that had delayed putting SCID on its newborn panel until the cost effectiveness of the rare condition — 1 in 50,000 births — was further studied.
“If we had been in Massachusetts or Wisconsin, Liam would have been tested at birth for SCID. If that had been the case, his journey, our journey may have had a different ending,” the Barretts said. “But he was born in the wrong state, Oregon.”
Oregon’s health panel recommended adding SCID to the newborn screen in 2014. But because its lab couldn’t immediately perform the analytical DNA testing, Oregon’s newborn screening samples for SCID were sent to Washington state’s lab. Within weeks, an Oregon baby was detected with SCID by Washington state lab technicians.
“We don’t screen for any condition we can’t treat,” said McCrillis. “But SCID is an example of how early detection works …. Casting our net really wide allows us to pick up these rare disorders and get the newborns the immediate attention that they need.”
My father used his own colorful cost-versus-benefit argument when persuading politicians and others to “do the right thing” and jab every newborn in the heel.
“A lot of politicians are beginning to be aware that it actually does save money to prevent non-lethal, lifelong handicapping conditions, because they require so damn much money,” he said in a 1980 article published in the Buffalo Courier-Express Sunday Magazine (my Dad appeared on the cover holding two babies.) He noted that costs to aid an individual with severe mental retardation added up to about $34,000 annually at a local center for the developmentally disabled. “You figure you save a million dollars every time you find a kid with PKU.”
My father did not receive royalties from his test, nor did he apply for a patent. He offered it in the name of public health and public service. He offered it in the name of his son and his niece, John and Margaret, and the thousands of yet unnamed children who would be spared from their same fate.
On June 28, my family and I and many organizations and individuals around the world, thanked my dad, Dr. Robert Guthrie, for his breakthrough discovery on what would have been his 100th birthday. He died in 1995. But you can hear his legacy every day in maternity hospitals the world over.
Patricia Guthrie is a freelance health reporter based in Shoreline.
She recently launched The Robert Guthrie Legacy Project to begin putting her father’s professional and personal archives online at http://www.robertguthriepku.org/
Talk to us
> Give us your news tips.
> Send us a letter to the editor.
> More Herald contact information.