Editorial: State, county overdose rates call for all-out effort
Published 1:30 am Saturday, August 26, 2023


By The Herald Editorial Board
It’s not that action hasn’t been taken, that laws and policies haven’t seen necessary change, that investments aren’t being made, but — as it takes any object with enough mass and inertia to be slowed and turned around — the pace of drug overdoses and deaths in Snohomish County and Washington state are not showing signs of reversing; or even so much as slowing.
The most recent data from national drug overdose death counts from the Centers for Disease Control and Prevention showed that overdose deaths in Washington state were growing at the highest percentage for all 50 states; to an estimated 3,024 deaths for a 12-month period as of March 2023 from 2,356 deaths in 12 months in March 2022, a 28% increase.
More alarming was that rate of overdose deaths in Snohomish County in 2020 — shown in data from the state Department of Health and shared in Snohomish County’s 2022 community health assessment — which was higher than that of the state; 28.3 deaths per 100,000 for the county, compared against 22.5 per 100,000 for the state.
Washington state does not have the highest per capita rate of overdose deaths in the nation; that’s a record that belongs to West Virginia, but the rate of overdose deaths there is falling, if slowly, nearly 2% in the past year.
No surprise, the problem is fentanyl. Primed by the oxycodone glut pushed by the Sackler family’s Purdue Pharma and other opioid makers during the last two decades, since 2021, synthetic opioids — specifically fentanyl, which is cheaper to produce and more deadly than other opioids — have accounted for nearly 90% of opioid deaths in the state, according to data from the University of Washington’s Addictions, Drug and Alcohol Institute.
What’s being done: The inertia driving overdoses and deaths is a bear, and their rise in the county and the state calls for even greater efforts and removal of barriers that are limiting the success of investments, changes to state law and the efforts of individuals and organizations invested in this fight.
A recounting of some of what has been done recently:
After the state Supreme Court threw out the state’s law on drug possession in 2021 — limiting the ability of police and prosecutors to intervene — the state Legislature this spring adopted a comprehensive change to state law that among several provisions made possession a gross misdemeanor, allowing police — especially those teamed with social workers — and prosecutors greater leverage to persuade those found in possession of drugs to seek treatment.
At the same time, Snohomish County Executive Dave Somers announced a two-pronged approach to addressing the fentanyl crisis, including an investment of $1.4 million from opioid lawsuit settlement funds, the first of $14 million that the county expects to receive over the next 15 years, part of the $518 million the state received in a settlement with pharmaceutical companies that manufactured and irresponsibly distributed prescription opioids.
That first tranche of funds will be used to expand access to Narcan, which can save lives by reversing overdoses; provide funding to community groups for their outreach and treatment efforts; and support education efforts to counter substance use disorder.
Earlier this spring the county also announced $8 million in federal funding for capital projects throughout the county to increase capacity for behavioral health and substance use disorder treatment.
Secondly, the plan directs the county’s Multi-Agency Coordination group, with representatives from the sheriff’s office, the county health department and human service providers to develop short- and long-term strategies to address overdose, public safety and property damage problems.
Additionally, there have been major investments in shelter and supportive housing by cities and the county, such as the county’s recent purchase of two hotels for supportive housing and the construction and operation of facilities such as Clare’s Place and Cocoon House’s Hub in Everett, among others.
Harm reduction: Key to slowing, then reversing the current rate of overdoses and deaths — and returning lives to health and happiness and communities to safety and productivity — will be harm reduction in the short-term and treatment for the long-term. The harm reduction — needle exchanges, availability of Narcan and other programs — comes first; treatment for addiction is no longer an option for those who haven’t survived a drug overdose.
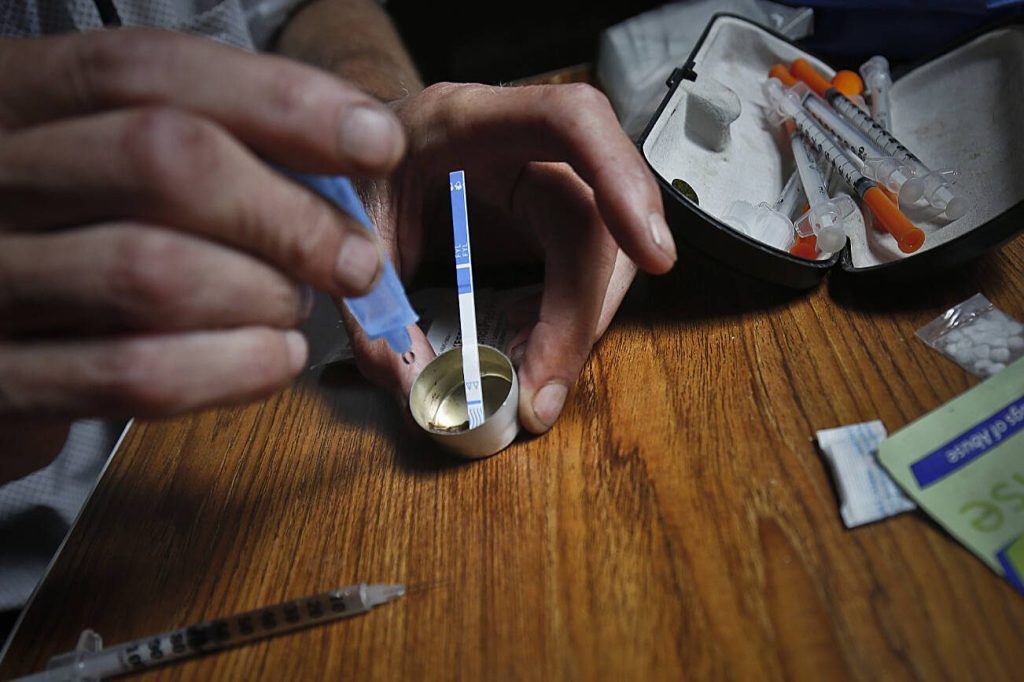
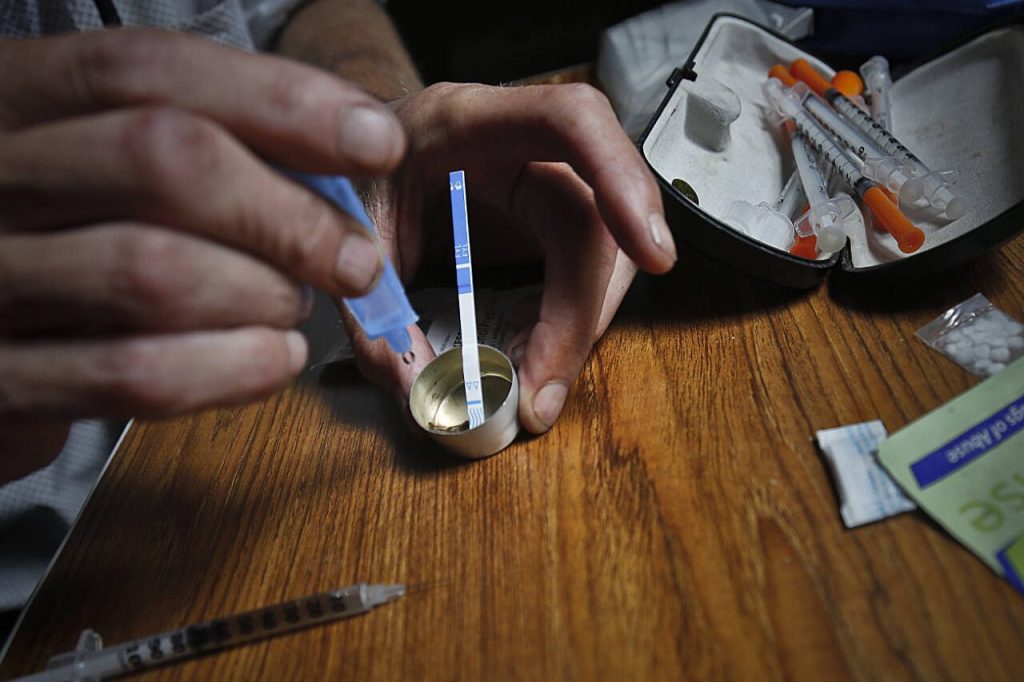
Among the other provisions in the changes made to state law this spring was removal of the drug paraphernalia tag from kits that can test drugs for the presence of fentanyl and xylazine, which is used legally as a veterinary anesthetic. Often, neither drug is purchased or otherwise obtained knowingly; it can be mixed with other drugs, such as in knock-off oxycodone pills, exposing people to the deadly synthetics at unknown dosages. The kits — strips that are exposed to a small amount of a drug mixed with water — can quickly test drugs, and allow users to avoid poisoning from fentanyl and xylazine.
A 2018 study by the Johns Hopkins Bloomberg School of Public Health and Rhode Island Hospital conducted interviews with people using drugs in three major East Coast cities. Of those, three-quarters said they believed they had unknowingly consumed fentanyl at least once and 85 percent of those said they wished they had known fentanyl was in the substance they used; 70 percent said that knowing their drugs contained fentanyl would lead them to modify their behavior.
Those kits are now legal and the state Department of Health is spending about $100,000 in the coming year to distribute about 75,000 fentanyl test strips. Snohomish County has received $125,000 from the state-supported North Sound Behavioral Health, part of which will be used to purchase an initial supply of 1,000 fentanyl and xylazine test strips. A distribution plan is being develeoped, said Kelsey Nyland, a spokeswoman for the county, which will supply efforts by the Snohomish County Outreach Team and distribution to youths, individuals at the county’s Carnegie Resource Center and Diversion Center and those newly enrolled in medication-assisted treatment.
Access to treatment is improving. Earlier this week, a new clinic offering medication treatment for opioid and other addictions — including buprenorphine, naltrexone and methadone, which relieves withdrawal and discourages drug use — was announced in south Everett at a former sandwich shop at 5130 Evergreen Way. Community Medical Services’ new clinic will expand the number of such clinics in Everett to three.
Push-back: Still that improvement in access to treatment services has seen some push-back. When an opioid treatment clinic, run by Acadia Healthcare, announced its state-approved move from Bothell to Lynnwood in January, activists in the city and the Lynnwood City Council objected to the clinic’s move, and in April the council adopted a six-month moratorium on such facilities.
When its moratorium expires, Lynnwood’s council should review its experience with the Acadia clinic thus far as well as its record in Bothell, and reconsider any past objections to facilities that in appearance and fit with the community are little different from a dentist’s office.
And in the same week that the new addiction treatment facility was announced in south Everett, a nonprofit behavioral health clinic, the Center for Human Services, intending to provide counseling for behavioral health and those with substance use disorders, learned it would have to cancel its plans to move to a downtown office on Colby Avenue because city policy — the city’s Metro Everett Plan — bars medical and social service facilities from ground-floor spaces in the downtown area. The city council passed the plan in 2018, intent on reserving space for residential and mixed-use development.
While the city’s vision for its downtown outlines desirable goals — and Everett shouldn’t have to shoulder an unreasonable share of social services in the county — there’s cause to allow for more flexibility within its Metro plan, keeping its guidelines but allowing a process for case-by-case consideration of some facilities.
There’s hope that the efforts listed above — along with many others — will help turn the tide against the rising threat of overdoses and deaths and return a greater level of safety and livability to the county and its cities.
We’ve yet to see that reflected in the grim numbers now confronting us.
More opportunities for programs and facilities will follow, often backed with the funding and experience necessary for success, but they will require the support and participation of communities and local officials.
With overdoses and deaths continuing to rise, every effort — every opportunity — must be employed to slow, then reverse these trends.