Hooked on hope, she chose behavioral therapy over law school
Published 1:30 am Tuesday, November 6, 2018




MARYSVILLE — Sally Anne Schneider, the new chief executive at Smokey Point Behavioral Hospital, credits her career choice to a nosy stranger at a Bellingham fish bar.
In 1984, Schneider, who had just earned a bachelor’s degree from Western Washington University, was discussing law school plans with a friend over lunch.
An attorney overheard the conversation and offered counsel. “Basically, he talked me out of going to law school,” Schneider said.
The chance encounter made Schneider rethink her career choice. She decided to pursue a master’s of science degree in marriage and family therapy.
“I always loved being a therapist,” she said. “You get to make an incredible difference in someone’s life.”
“So much of mental health is about hope,” said Schneider, 56, who was raised in St Louis and attended WWU in Bellingham.
“I got an exceptional education there,” she said.
Two months ago, she returned to the Northwest to lead the new Smokey Point Hospital. The hospital, which opened in June 2017, has been in start-up mode, she said. Now the priority is creating and maintaining a stable staff.
The psychiatric hospital provides mental health services and addiction treatment for children and adults. The 115-bed facility at 3955 156th St. NE in Marysville offers inpatient and outpatient care.
It’s owned by US HealthVest, which also operates mental health facilities in Illinois, Georgia and, now, Washington.
The company plans next year to open a psychiatric hospital in Lacey, its second location in this state.
Schneider replaces former CEO Matt Crocker, who resigned during the summer.
Previously she was CEO of LifeCare Behavioral Health Hospital in Pittsburgh. Before that, she was chief behavioral health officer at Bartlett Regional Hospital in Juneau, Alaska.
The Smokey Point hospital is a welcome addition to the region, said Lisa Utter, executive director of the Snohomish County chapter of the National Alliance on Mental Illness (NAMI).
“North Snohomish County really needed additional capacity,” Utter said.
The NAMI chapter holds a support group at the hospital on Wednesdays that is open to anyone, Utter said. “They’ve been very supportive of us,” she said of Smokey Point Behavioral Hospital.
When plans for a psychiatric hospital in Snohomish County were announced in 2013, the county’s only inpatient psychiatric unit was at Swedish/Edmonds, a 23-bed facility that treats only adults. The closest inpatient facilities for children and adolescents were Fairfax Hospital in Kirkland, with 15 beds, and Seattle Children’s Hospital, with 20.
The Smokey Point hospital cares for patients with thoughts of harming themselves or others, severe depression, post-traumatic stress disorder and people who need treatment for both mental health issues and drug or alcohol problems, said Alicia Jacobs, the hospital’s community liaison.
Patients can stay up to 14 days. Longer stays can also be arranged.
The hospital can treat up to 14 patients ages 13 to 17 and “12-year-olds on a case-by-case basis,” Jacobs said.
A social worker from the hospital has begun making weekly visits to high schools in the Arlington and Lakewood districts at no cost to them.
Families can call the hospital day or night for free guidance on whether a child needs to be hospitalized, Jacobs said.
“We’re particularly happy about their adolescent services,” Utter said.
Location is everything, Schneider said.
When a hospital is in the community it serves, families are more likely to visit and be involved in care, she said.
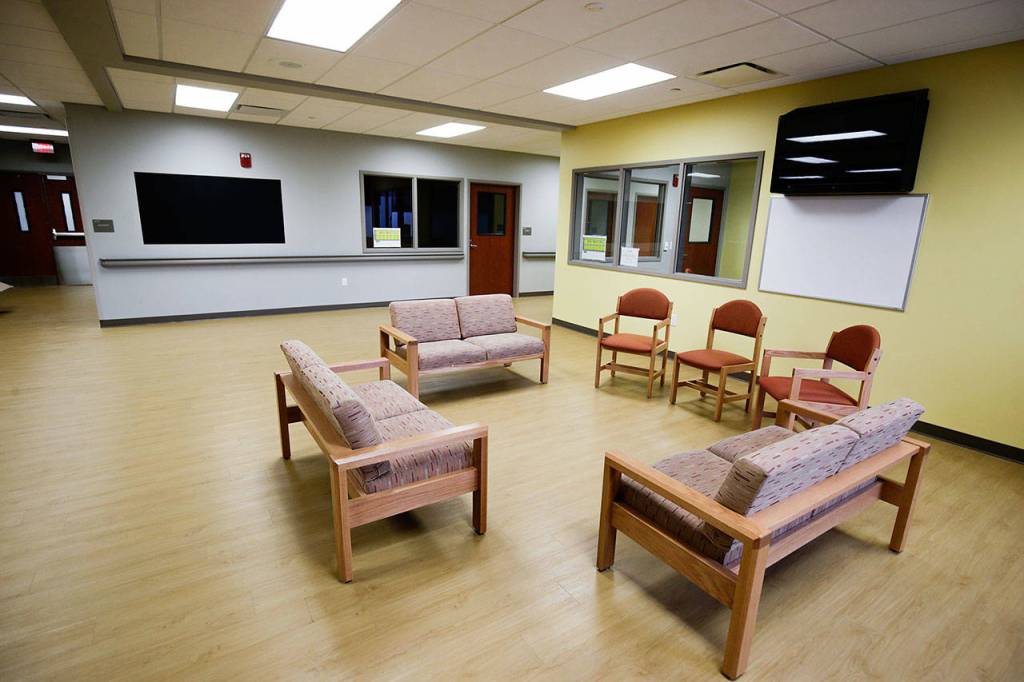
“The building itself is beautiful,” Schneider said.
The hospital’s interior blends cool blue and burnt-orange walls with wood floors. Patient rooms are small and bright, like a new college dormitory.
A small indoor gym features a stair-stepper, stationary bicycle and other exercise equipment.
Patients are treated in separate groups, depending on their age, background or the issues they’re facing.
For example, the hospital has a unit specializing in mental health care for those in the military — the only program of its kind in Washington.
The needs of traumatized women, for example, are different than those of active-duty military personnel experiencing post-traumatic stress disorder.
“Members of a women’s group may be less trusting and more fear-based,” she said. Establishing a safe environment is a key part of treatment.
Schneider hopes to expand inpatient youth services and raise the adolescent unit’s capacity to 20 patients.
Utter, head of the local NAMI chapter, said some community members are concerned that the hospital hasn’t gotten up to speed as quickly as hoped.
The hospital had planned to have all 115 beds available within eight months.
It’s currently operating at about 75 to 85 percent of capacity.
“They’ve acknowledged having difficulty in staffing to full capacity,” said Utter.
US HealthVest’s chief executive officer, Dr. Robert Kresch, said that staffing issues are to be expected at this early stage. Kresch spent 20 years as a psychiatrist at Columbia Presbyterian Medical Center in New York.
“It’s hard work to open a hospital and get it competent and trained permanent staff,” he said. “In the early days you expect a fair amount of turnover.”
Schneider’s plans including hiring a chief of nursing, a nursing director and an educator.
On her wish list: Partnering with local colleges and universities.
“I want us to have internships and training sites for our local universities, and hopefully take psychiatric residents” from medical schools, she said.
On a personal note, Schneider looks forward to her own family moving here next spring from Pittsburgh. She has a husband and a son.
As for the Bellingham attorney, Schneider thinks she’s identified him.
“I’ve got to get up there and thank him,” she said.
Janice Podsada; jpodsada@heraldnet.com; 425-339-3097; Twitter: JanicePods