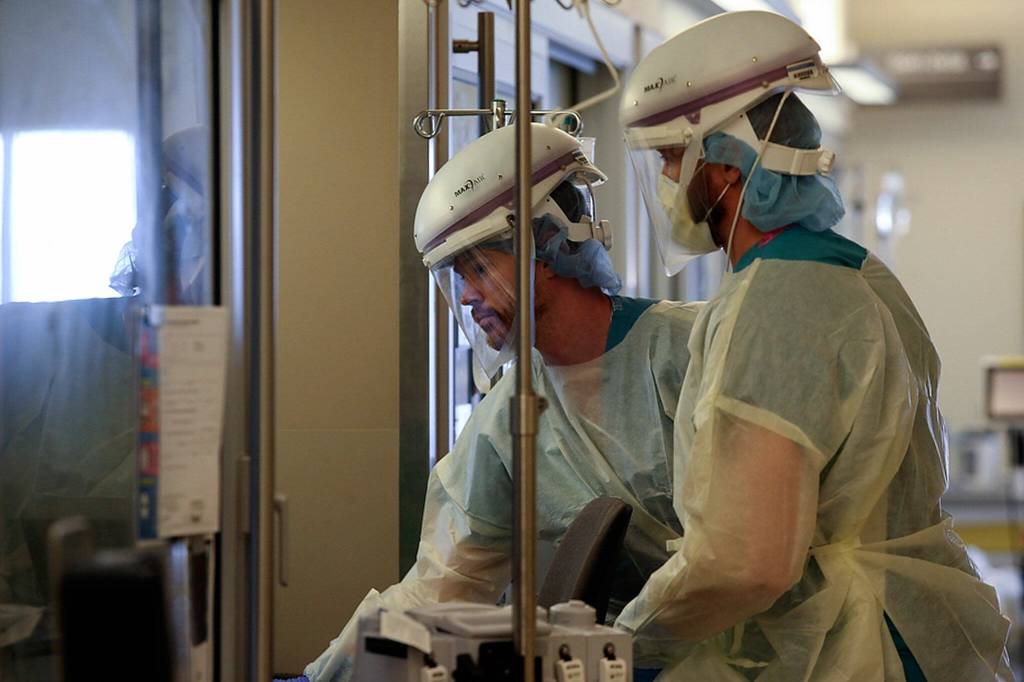
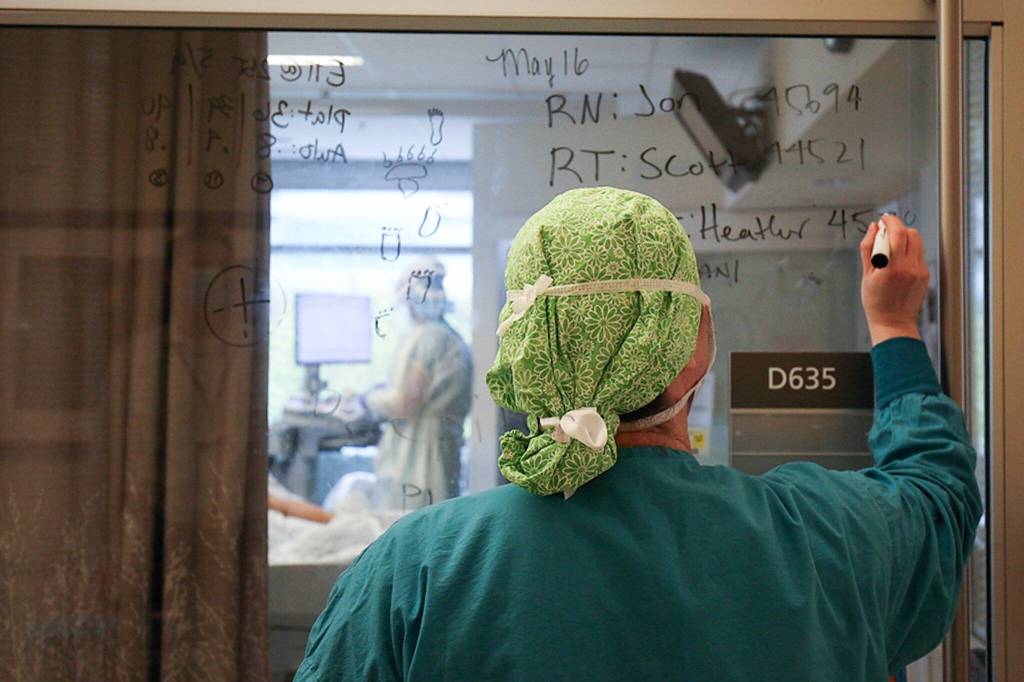
‘Few core staff left’: Droves of nurses take high-paying travel jobs
Published 1:30 am Monday, January 31, 2022





ARLINGTON — After nine years at Providence Regional Medical Center Everett, Cecillia Hoglund said she’s finally joining the “bandwagon.” The ICU nurse is leaving her post to become a travel nurse.
On travel contracts, Hoglund expects to make $4,500 a week. That’s about four times what she made at Providence. Despite the title, she’ll likely stay in state, at another facility in Western Washington.
And she hopes it will help her “emotionally endure.” Before the pandemic, Hoglund felt like her work in the ICU meant the difference between a patient dying — what she calls a “celestial discharge” — or a patient getting better. Now, she said, fewer and fewer of her patients recover.
“To be frank, I’m shoveling people into body bags faster than they can keep them stocked,” she told The Daily Herald. “You’re holding an iPad in all your gear and you’re crying to yourself because there’s a wailing family member on an iPad crying and saying goodbye while you’re holding the patient’s hand.”
Travel nursing is a field that has boomed in the past two years, with demand up for short-term positions, and those who fill them enjoying significantly higher wages.
More nurses are making the same choice. Hoglund estimated her Providence unit was about 80% travel nurses when she left this month.
“There’s very few core staff left,” she said. “Since COVID we’ve been getting droves and droves and droves of travelers.”
‘Not sustainable’
The situation was made worse this winter, when omicron flooded hospitals with record numbers of COVID hospitalizations. In Snohomish County, the figure peaked around 200, prompting a deployment of the Washington National Guard to Providence.
The Everett hospital confirmed this month that more of the temporary positions have been brought on amid the pandemic. But staff and officials say they can’t rely on travel nurses forever.
It’s “not a desirable or sustainable approach,” Providence spokesperson Casey Calamusa wrote in an email to The Herald.
As of last November, hospitals around the state were using nearly 3,000 travel nurses, according to the Washington State Hospital Association, which also called the approach “not sustainable.” The time it takes to fill a registered nurse vacancy rose 54% from 2019 to 2021, with well-documented burnout precipitating what officials have deemed the “great resignation.”
In some ways, the use of travel nurses has created a feedback loop within hospitals. The presence of so many short-term, highly paid nurses can frustrate in-house staff, exacerbating the burnout that led to high travel nurse demand in the first place.
Everett emergency department nurse Matthew Deitz, for example, said he wants to hold onto his job. But it’s hard seeing so many of his coworkers walk away and be replaced by travel nurses. There are some “key people” he loves working with. If they leave the hospital for travel positions, he would consider it, too.
“I keep an open mind to it,” he said. “I’ve been with Providence for 11 years, so I do feel loyalty to this hospital.”
For Hoglund, spending her shifts answering “a million questions from a traveler who’s making four times what I’m making — it’s frustrating.”
It’s hard to form meaningful connections with coworkers who only stay for a few weeks or months. After performing back-to-back CPR on patients, she said, it’s nice if a long-time coworker asks how she’s doing, emotionally.
“Those dynamics are kind of missing now,” she said. “That’s why I decided to finally leave.”
‘Headhunters’
An analysis of 2021 exit interviews by the Washington State Hospital Association found 15% of nurses were pursuing travel nurse gigs. That was the third-most cited reason for leaving, behind a spouse’s relocation (16%) and other unspecified reasons (27%).
It means booming business for agencies working to fill in the gaps.
This month AMN Healthcare Services, the nation’s largest temporary staffing company, said last quarter’s revenue exceeded earlier estimates by $70 million, with demand at “record levels.” A presentation to investors cited “significant opportunity with a large, fragmented market,” pointing to a projected shortage of physicians to reach 139,000 by 2033, with the pandemic accelerating turnover. Revenue this quarter was expected to surpass $1.1 billion.
Michael Colosi, an executive at NSI Nursing Solutions, said the “incredible” surge in travel nurse demand can’t be sustained for long, as hospitals shell out big bucks for short contracts. He described hospitals spending hundreds of thousands of dollars a year for the equivalent of one full-time employee.
“I mean, that’s what you pay a surgeon,” Colosi said.
That’s where NSI Nursing Solutions comes in. The company finds and places permanent staff with hospitals. They generally get paid less than travel nurses, but still more than their new coworkers.
“We are, for lack of a better term, headhunters,” Colosi said.
As for the tension that arises from pay gaps, he said, “that’s inherent in any business. It’s just been more polarized right now.”
For Deitz, the trend is worrisome. What was meant to be a short-term solution now seems like the norm.
“I saw this happening over a year ago as people slowly started to leave. Eventually everyone’s going to want to travel,” he said. “It’s eventually going to come to a head.”
‘Always in the air’
Some states have already moved to restrict how much registered nurses could be paid in certain situations. In Pennsylvania, Republican lawmakers are backing a bill that would regulate contract health care agencies and prohibit them from charging more than 150% of a nursing home’s average rate.
Massachusetts and Minnesota also have some restrictions on how much agencies can charge nursing homes for temporary staff.
In Washington, Gov. Jay Inslee said this week that wage caps aren’t the solution.
“We need more nurses. It’s pretty simple,” he said. “… We are on both ends of this challenge. So we’re using traveling nurses and therefore competing against ourself.”
Inslee cited his proposal to invest millions into residency programs, expanding them with the aim of bulking up the workforce.
In the meantime, young resident nurses entering a field where morale is low, with no end in sight.
One recent nursing school graduate told The Daily Herald she noticed the general mood at Providence is, “I don’t know how much longer I can do this.”
“It feels like it’s always in the air,” said the nurse, who asked to remain anonymous out of concern for her new job. “… Especially on a really bad night, even with mentors I really look up to, who have been at Providence for 10 or more years.”
The employee said there’s a definite stigma around travel nurses and how much they get paid.
But as she cares for five to six patients each night, she appreciates — and needs — the help.
“I’d just be happy,” she said, “to have more staff and less pressure on me.”
Claudia Yaw: 425-339-3449; claudia.yaw@heraldnet.com. Twitter: @yawclaudia.